Can pericarditis lead to myocarditis
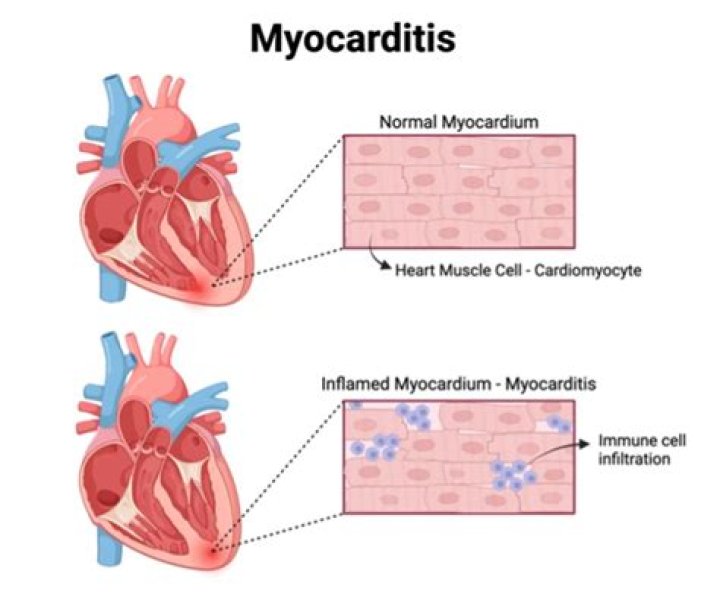
As is the case with pericarditis, viruses are the most common causative agents in myocarditis, but the cause can also be bacterial, fungal, or noninfectious. The clinical presentation of myocarditis can range from minor chest pain to cardiogenic shock.
Does pericarditis cause myocarditis?
Myocarditis is different than pericarditis. Pericarditis is an inflammation of the sac that surrounds the heart (pericardium) and not the heart muscle itself. However, it is not unusual to have a patient present with both pericarditis and myocarditis.
What can pericarditis lead to if untreated?
Pericarditis may result in one of two serious complications: cardiac tamponade and chronic constrictive pericarditis. Cardiac tamponade is considered a medical emergency and, if left untreated, can quickly become fatal. It develops when too much fluid builds up between the heart muscle (myocardium) and the pericardium.
What does pericarditis lead to?
Some people with long-term (chronic) pericarditis develop permanent thickening and scarring of the pericardium, which prevents the heart from filling and emptying properly. This unusual complication often leads to severe swelling of the legs and abdomen and shortness of breath.How do you test for myocarditis pericarditis?
- Electrocardiogram (ECG or EKG). This quick and painless test shows your heart’s electrical patterns and can detect irregular heartbeats.
- Chest X-ray. …
- Heart MRI (Cardiac MRI ). …
- Echocardiogram. …
- Blood tests. …
- Cardiac catheterization and heart muscle biopsy.
How do you treat myocarditis or pericarditis?
Treatment. If you are diagnosed with heart inflammation such as endocarditis, myocarditis, or pericarditis, your doctor may recommend medicine or surgery to treat your condition. Mild cases of myocarditis and pericarditis may go away without treatment.
Do I have pericarditis or myocarditis?
Myocarditis is inflammation of the heart muscle, and pericarditis is inflammation of the outer lining of the heart. In both cases, the body’s immune system causes inflammation in response to an infection or some other trigger.
What are the potential risk factors for pericarditis?
- A past heart attack.
- Autoimmune diseases.
- Trauma or injury from an accident.
- Certain bacterial, viral and fungal infections.
- Kidney failure.
- Rarely, certain medications such as phenytoin to treat seizures and procainamide to treat irregular heartbeats.
Is pericarditis an autoimmune disease?
Recurrent pericarditis, like chronic myocarditis, is often considered to be an autoimmune consequence of a prior viral infection.
What can mimic pericarditis?In addition to these conditions, chest pain that can mimic pericarditis is seen in a wide range of conditions including gastric inflammation (gastritis) or ulcers, esophageal inflammation (esophagitis) and gastroesophageal reflux disease (GERD), clots in the arteries of the lung (pulmonary embolism), inflammation of …
Article first time published onCan you have pericarditis for years?
Pericarditis is usually acute – it develops suddenly and may last up to several months. The condition usually clears up after 3 months, but sometimes attacks can come and go for years. When you have pericarditis, the membrane around your heart is red and swollen, like the skin around a cut that becomes inflamed.
How long can you live with pericarditis?
Long-term survival after pericardiectomy depends on the underlying cause. Of common causes, idiopathic constrictive pericarditis has the best prognosis (88% survival at 7 years), followed by constriction due to cardiac surgery (66% at 7 years).
Is pericarditis life long?
Pericarditis can be acute or chronic. “Acute” means that it occurs suddenly and usually doesn’t last long. “Chronic” means that it develops over time and may take longer to treat. Both acute and chronic pericarditis can disrupt your heart’s normal rhythm and/or function and possibly (although rarely) lead to death.
What is worse pericarditis or myocarditis?
The clinical presentation of myocarditis can range from minor chest pain to cardiogenic shock. Indeed, myocarditis is associated with more serious long-term sequelae than pericarditis is, the most serious of which are dilated cardiomyopathy and heart failure.
Can you see myocarditis on Echo?
It is concluded that echocardiographic features of myocarditis are polymorphous and nonspecific. The echocardiographic pattern can simulate alternatively dilated, hypertrophic, restrictive or “right” ventricular cardiomyopathy, as well as coronary artery disease.
Does pericarditis show on ECG?
The electrocardiogram (ECG) is very useful in the diagnosis of acute pericarditis. Characteristic manifestations of acute pericarditis on ECG most commonly include diffuse ST-segment elevation. However, other conditions may have ECG features similar to those of acute pericarditis.
What viral infection causes pericarditis?
The following viral infections can lead to pericarditis: Usual viral and cold meningitis caused by a group of viruses (enteroviruses) Glandular fever. Pneumonia and bronchitis caused by adenoviruses.
Can blood test detect myocarditis?
There are no specific blood tests to confirm the diagnosis of myocarditis; however, an otherwise unexplained elevation in troponin (a blood test that indicates heart muscle damage) and/or electrocardiographic features of cardiac injury are supportive.
Why do I keep getting pericarditis?
Causes of pericarditis The cause of pericarditis is often unknown, though viral infections are a common reason. Pericarditis may occur after a respiratory or digestive system infection. Chronic and recurring pericarditis may be caused by autoimmune disorders such as lupus, scleroderma and rheumatoid arthritis.
Can you get pericarditis twice?
Recurring (or relapsing) pericarditis may be intermittent or constant. The first recurrence is usually within 18 to 20 months of the initial attack. Pericarditis is considered chronic when a relapse occurs as soon as anti-inflammatory treatment is stopped.
Can pericarditis flare up?
The pericardial sac becomes scarred and stiff, limiting the heart’s pumping action. This can occur in someone during the first (acute) episode or after recurrent (repeat) pericarditis flares. In some cases of constrictive pericarditis, the pericardium may need to be partially or completely removed.
Can pericarditis resolve itself?
Pericarditis is often mild and goes away on its own. Some cases, if not treated, can lead to chronic pericarditis and serious problems that affect your heart. It can take weeks or months to recover from pericarditis.
What does myocarditis do to the heart?
Myocarditis occurs when the heart muscle becomes inflamed. When your heart muscle is inflamed, it can affect your heart’s electrical system. This can cause arrhythmia, or a rapid or abnormal heartbeat. Myocarditis can cause the heart muscle to weaken and can lead to cardiomyopathy.
Does pericarditis show on cardiac MRI?
Although cardiac MRI appears to be useful in detecting pericardial inflammation, the imaging studies have not had direct confirmation with histologic data. Since pericarditis is usually not associated with mortality, autopsy correlation with pre-mortem MRI imaging is non-existent.
Is there a blood test for pericarditis?
Blood tests are usually done to check for signs of a heart attack, inflammation and infection. Other tests used to diagnose pericarditis include: Electrocardiogram (ECG).
What is complicated pericarditis?
Although most patients with acute pericarditis will have resolution, some will develop incessant, recurrent, chronic, or constrictive pericarditis. Many of these patients experience a debilitating chronic disease, and to simplify presentation throughout this review, are referred to as having complicated pericarditis.
Is walking good for pericarditis?
In conclusion, pericarditis is a common inflammatory condition of the pericardium with multiple etiologies. Current guidelines recommend restriction of intense physical activity and return to activity once there is no evidence of active inflammation.
Does pericarditis get worse with exercise?
Studies have also reported a relationship between pericarditis and genetic variations of the immune system that can predispose people to worsening inflammation from environmental triggers such as exercise [15].