How do you diagnose dyslipidemia
Dyslipidemia is diagnosed by measuring serum lipids. Routine measurements (lipid profile) include total cholesterol (TC), TGs, HDL cholesterol, and LDL cholesterol.
What is the difference between high cholesterol and dyslipidemia?
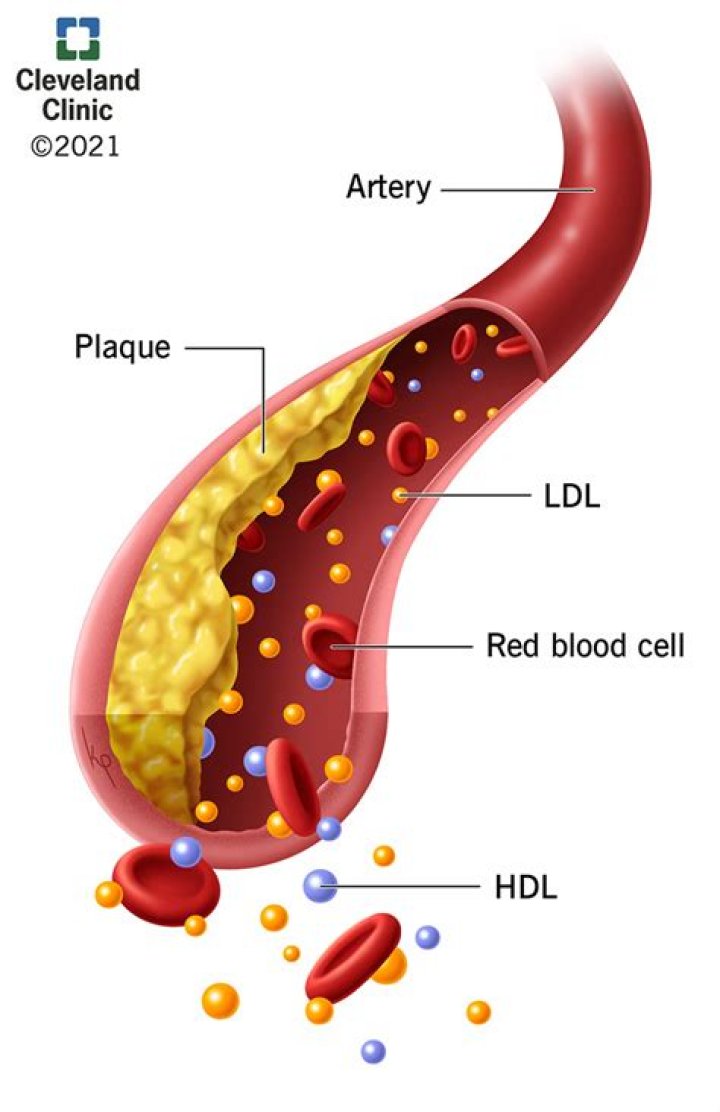
If you have dyslipidemia, it usually means your LDL levels or your triglycerides are too high. It can also mean your HDL levels are too low. LDL cholesterol is considered the “bad” type of cholesterol. That’s because it can build up and form clumps or plaques in the walls of your arteries.
What is the main cause of dyslipidemia?
Dyslipidemia is classified into primary and secondary dyslipidemia. Primary causes are single or multiple gene mutations that result in either overproduction or defective clearance of triglycerides (TG) and low-density lipoprotein (LDL), or in underproduction or excessive clearance of high-density lipoprotein (HDL).
How is dyslipidemia defined?
Dyslipidemia, defined as elevated total or low-density lipoprotein (LDL) cholesterol levels, or low levels of high-density lipoprotein (HDL) cholesterol, is an important risk factor for coronary heart disease (CHD) and stroke.When can dyslipidemia be diagnosed?
For screening of dyslipidemia, all adults aged ≥ 21 years and younger individuals with other risk factors, such as a family history of premature CVD and severe dyslipidemia, should undergo a fasting lipid test every 4 to 6 years to assess total cholesterol, triglyceride, HDL-C, LDL-C (calculated using the Friedewald …
Can dyslipidemia be reversed?
Hyperlipidemia is treatable, but it’s often a life-long condition. You’ll need to watch what you eat and also exercise regularly. You might need to take a prescription medication, too. The goal is to lower the harmful cholesterol levels.
How do you treat dyslipidemia naturally?
In dyslipidemia especially in older or disabled individuals, increasing physical activity for more than 30 minutes for 5 days a week, moderate-intensity aerobic exercise [19], and high-intensity resistance exercises can all reduce LDL and triglycerides and increase HDL [20].
Can dyslipidemia cause hypertension?
Dyslipidemia, a strong predictor of cardiovascular disease,5 causes endothelial damage,6–8 and the loss of physiological vasomotor activity that results from endothelial damage may become manifested as increased blood pressure (BP).What is primary prevention for dyslipidemia?
Guidelines across the globe recommend lipid lowering treatment, for which statins are the cornerstone pharmacotherapy, for primary prevention in patients with elevated baseline cardiovascular risk.
What foods cause dyslipidemia?Although dyslipidemia is commonly addressed with statins, it is important for patients to understand that lipid abnormalities are not caused by a “statin deficiency.” Rather, they are usually the result of dietary factors, particularly the inclusion of dairy products, meat, eggs, and hydrogenated oils and the absence …
Article first time published onWhat is the difference between hypertriglyceridemia and dyslipidemia?
When triglycerides are only affected, this may be referred to as hypertriglyceridemia (high triglyceride levels) or hypotriglyceridemia (low triglyceride levels). Conversely, if an individual has both triglyceride and cholesterol levels affected, this is referred to as a “combined” or “mixed” dyslipidemia.
What drug classes are used for dyslipidemia?
The most commonly used options for the pharmacologic treatment of dyslipidemia are statins, resins, fibrate, niacin, and their combinations.
What blood test shows hyperlipidemia?
Hyperlipidemia has no symptoms, so the only way to detect it is to have your doctor request a blood test called a lipid panel or a lipid profile. Your doctor will use your lipid panel to make a hyperlipidemia diagnosis. This test determines your cholesterol levels.
When should you start treatment for dyslipidemia?
Dietary therapy should be initiated in patients who have borderline-high LDL cholesterol levels (130 to 159 mg per dL [3.35 to 4.10 mmol per L]) and two or more risk factors for coronary heart disease and in patients who have LDL levels of 160 mg per dL (4.15 mmol per L) or greater.
What is the fastest way to lower LDL cholesterol?
- Reduce saturated fats. Saturated fats, found primarily in red meat and full-fat dairy products, raise your total cholesterol. …
- Eliminate trans fats. …
- Eat foods rich in omega-3 fatty acids. …
- Increase soluble fiber. …
- Add whey protein.
What's the best supplement for high cholesterol?
Niacin. Niacin is a B vitamin. Doctors sometimes suggest it for patients with high cholesterol or heart concerns. It increases the level of good cholesterol and reduces triglycerides, another fat that can clog arteries.
What is the fastest way to lower cholesterol without medication?
- Avoid trans and saturated fats. …
- Eat lots of soluble fiber. …
- Exercise. …
- Cut down on your alcohol intake. …
- Try fish oil supplements. …
- Take a garlic supplement.
What is mild hyperlipidemia?
Hyperlipidemia means your blood has too many lipids (or fats), such as cholesterol and triglycerides. One type of hyperlipidemia, hypercholesterolemia, means you have too much non-HDL cholesterol and LDL (bad) cholesterol in your blood. This condition increases fatty deposits in arteries and the risk of blockages.
What is the life expectancy of someone with familial hypercholesterolemia?
Familial hypercholesterolemia FAQs A: Without treatment, the life expectancy of those with familial hypercholesterolemia can be reduced by approximately 15-30 years. However, in people with homozygous familial hypercholesterolemia, the life expectancy may only be 20 years or less.
Can low LDL reverse heart disease?
“These patients are two to four times more likely than people without diabetes to die from heart disease. For the first time, we have evidence that aggressively lowering LDL cholesterol and blood pressure can actually reverse damage to the arteries in middle-aged adults with diabetes.”
What is secondary prevention of dyslipidemia?
Cardiovascular disease is the leading cause of death in women and the treatment of dyslipidemia is a cornerstone of secondary prevention. Pharmacologic therapy with statins can lower LDL-C by 30-50% and reduce the risk of recurrent coronary heart disease in both men and women.
Can dyslipidemia cause diabetes?
Dyslipidemia is one of the major risk factors for cardiovascular disease in diabetes mellitus. The characteristic features of diabetic dyslipidemia are a high plasma triglyceride concentration, low HDL cholesterol concentration and increased concentration of small dense LDL-cholesterol particles.
Is hyperlipidemia a disease?
Hyperlipidemia is a major risk factor for heart disease. It refers to excess levels of LDL cholesterol and triglycerides in the blood. Doctors consider low-density lipoprotein (LDL) as bad cholesterol and high-density lipoprotein (HDL) as good cholesterol.
What can be prescribed for hyperlipidemia?
- HMG-CoA Reductase Inhibitors (Statins)
- Niacin (Nicotinic Acid)
- Fibric Acid Derivatives (Fibrates)
- Bile Acid Sequestrants.
- Combination Therapy and Compliance.
What is the first line drug for hyperlipidemia?
HMG-CoA reductase inhibitors, or statins, are the recommended first-line therapy for most patients. These are the most prescribed drugs in the world and are considered the most effective lipid-lowering agents available, both in lowering LDL-C levels and in the prevention of CV events.
Why lipid profile test is done?
why get tested? The lipid profile test is needed to check for dyslipidaemia symptoms, it is also carried out to check adults and children who are risk prone to high blood cholesterol value and triglycerides. This happens because of development of diabetes, high blood pressure or a heart disease.
Why lipid profile test is done in fasting?
Lipids have traditionally been drawn after a fast for two main reasons. The first was to minimize variation, since eating can affect some lipid levels. The second was to produce a better calculation of LDL-cholesterol, which is often derived from an equation thought to provide highly distorted results after eating.
Is lipid profile done fasting?
In most cases, you need to fast for 10 to12 hours before your lipid panel blood test. Fasting means not eating or drinking anything except water. In some cases, getting a lipid panel test without fasting is possible.
How often should lipids be checked on statin?
The ATP III recommendations for monitoring of statin therapy are as follows: check lipid panel at baseline, 6–8 weeks after starting or adjusting the medication/dose, and then every 4–6 months; check LFTs at baseline, approximately 12 weeks after starting therapy, then annually or more frequently if indicated; and …

