How is ventilator connected
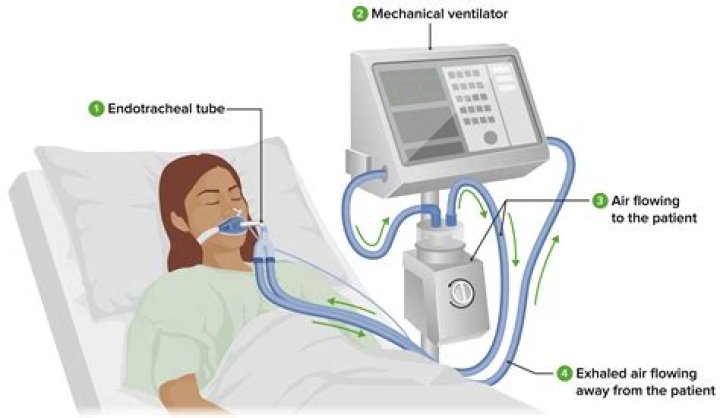
Some people may need to be on a ventilator for a few hours, while others may require one, two, or three weeks. If a person needs to be on a ventilator for a longer period of time, a tracheostomy may be required. During this procedure, a surgeon makes a hole in the front of the neck and inserts a tube into the trachea.
How long does someone typically stay on a ventilator due to COVID-19?
Some people may need to be on a ventilator for a few hours, while others may require one, two, or three weeks. If a person needs to be on a ventilator for a longer period of time, a tracheostomy may be required. During this procedure, a surgeon makes a hole in the front of the neck and inserts a tube into the trachea.
What are symptoms of COVID-19 affecting the lungs?
Some people may feel short of breath. People with chronic heart, lung, and blood diseases may be at risk of severe COVID-19 symptoms, including pneumonia, acute respiratory distress, and acute respiratory failure.
When do patients need ventilators to help treat COVID-19?
For the most serious COVID-19 cases in which patients are not getting enough oxygen, doctors may use ventilators to help a person breathe. Patients are sedated, and a tube inserted into their trachea is then connected to a machine that pumps oxygen into their lungs.What is the recovery time for COVID-19 patients with Acute Respiratory Distress Syndrome (ARDS)?
Most people who survive ARDS go on to recover their normal or close to normal lung function within six months to a year. Others may not do as well, particularly if their illness was caused by severe lung damage or their treatment entailed long-term use of a ventilator.
What happens to your lungs if you get a critical case of COVID-19?
In critical COVID-19 — about 5% of total cases — the infection can damage the walls and linings of the air sacs in your lungs. As your body tries to fight it, your lungs become more inflamed and fill with fluid. This can make it harder for them to swap oxygen and carbon dioxide.
Do all patients with COVID-19 get pneumonia?
Most people who get COVID-19 have mild or moderate symptoms like coughing, a fever, and shortness of breath. But some who catch the new coronavirus get severe pneumonia in both lungs. COVID-19 pneumonia is a serious illness that can be deadly.
When is remdesivir prescribed to COVID-19 patients?
Remdesivir injection is used to treat coronavirus disease 2019 (COVID-19 infection) caused by the SARS-CoV-2 virus in hospitalized adults and children 12 years of age and older who weigh at least 88 pounds (40 kg). Remdesivir is in a class of medications called antivirals.For which COVID-19 patients has been approved Remdesivir?
On October 22, 2020, the FDA approved the antiviral drug Veklury (remdesivir) for use in adults and pediatric patients (12 years of age and older and weighing at least 40 kg) for the treatment of COVID-19 requiring hospitalization.
What are the most used breathing aid devices for COVID-19?Breathing aid devices are used to support the patients who have acute respiration problem due to pneumonia associated diseases like COVID-19, asthma, and dry coughing. The most used devices which are utilized for COVID-19 treatment are oxygen therapy device, ventilator, and CPAP device.
Article first time published onCan the coronavirus disease cause breathing problems?
COVID-19 is a respiratory disease, one that especially reaches into your respiratory tract, which includes your lungs. COVID-19 can cause a range of breathing problems, from mild to critical.
Is COVID-19 lung damage reversible?
After a serious case of COVID-19, a patient’s lungs can recover, but not overnight. “Recovery from lung damage takes time,” Galiatsatos says. “There’s the initial injury to the lungs, followed by scarring.
Can COVID-19 cause acute respiratory distress syndrome?
Lung damage in the course of this disease often leads to acute hypoxic respiratory failure and may eventually lead to acute respiratory distress syndrome (ARDS). Respiratory failure as a result of COVID-19 can develop very quickly and a small percent of those infected will die because of it.
Is COVID-19 linked to acute respiratory distress syndrome (ARDS) and multi-organ dysfunction?
The significant mortality rate associated with the ongoing Coronavirus disease 2019 (COVID-19) pandemic has been linked to acute respiratory distress syndrome (ARDS) and multi-organ dysfunction. Mechanisms underlying the phenomenon remain unclear.
Can COVID-19 spread through HVAC systems?
While airflows within a particular space may help spread disease among people in that space, there is no definitive evidence to date that viable virus has been transmitted through an HVAC system to result in disease transmission to people in other spaces served by the same system.
Can fans be used to decrease the risk of COVID-19 transmission indoors?
Yes. While fans alone cannot make up for a lack of outdoor air, fans can be used to increase the effectiveness of open windows, as described in the CDC list of ventilation improvement considerations.
Which organ system is most often affected by COVID-19?
COVID-19 is a disease caused by SARS-CoV-2 that can trigger what doctors call a respiratory tract infection. It can affect your upper respiratory tract (sinuses, nose, and throat) or lower respiratory tract (windpipe and lungs).
What are the odds of getting severe COVID-19 symptoms?
Most people will have mild symptoms and get better on their own. But about 1 in 6 will have severe problems, such as trouble breathing. The odds of more serious symptoms are higher if you’re older or have another health condition like diabetes or heart disease.
Can COVID-19 cause severe organ damage?
Led by researchers from NYU Grossman School of Medicine, the study revealed the protein signals given off by platelets—cell fragments that contribute to blood clotting—create inflammation, abnormal clotting, and damage to vessels when exposed to the pandemic virus.
Is shortness of breath an early symptom of Pneumonia due to COVID-19?
Breathlessness is caused by an infection in the lungs known as pneumonia. Not everyone with COVID-19 gets pneumonia, though. If you don’t have pneumonia, you probably won’t feel short of breath.
What are some of the common symptoms of the COVID-19 disease?
Symptoms may include: fever or chills; cough; shortness of breath; fatigue; muscle and body aches; headache; new loss of taste or smell; sore throat; congestion or runny nose; nausea or vomiting; diarrhea.
What happens to the body during a COVID-19 critical infection?
During a severe or critical bout with COVID-19, the body has many reactions: Lung tissue swells with fluid, making lungs less elastic. The immune system goes into overdrive, sometimes at the expense of other organs. As your body fights one infection, it is more susceptible to additional infections.
Why a ventilator is needed during the COVID-19 pandemic?
When your lungs inhale and exhale air normally, they take in oxygen your cells need to survive and expel carbon dioxide. COVID-19 can inflame your airways and essentially drown your lungs in fluids. A ventilator mechanically helps pump oxygen into your body.
Why do some people with COVID-19 need ventilators to breath?
When your lungs inhale and exhale air normally, they take in oxygen your cells need to survive and expel carbon dioxide. COVID-19 can inflame your airways and essentially drown your lungs in fluids. A ventilator mechanically helps pump oxygen into your body.
Is Redemsvir a drug for treating COVID-19?
Remdesivir is an FDA-approved (and sold under the brand name Veklury) intravenous antiviral drug for use in adult and pediatric patients 12 years of age and older and weighing at least 40 kilograms (about 88 pounds) for the treatment of COVID-19 requiring hospitalization.
Is Remdesivir approved in Europe for treatment of COVID-19?
Since July 2020, remdesivir has been conditionally approved in Europe for the treatment of coronavirus disease (COVID-19) in adults and adolescents aged 12 years and older with pneumonia who require supplemental oxygen but no invasive ventilation.
What is Remdesivir?
Remdesivir is in a class of medications called antivirals. It works by stopping the virus from spreading in the body.
How long does it take to recover from COVID-19?
Fortunately, people who have mild to moderate symptoms typically recover in a few days or weeks.
Which medications can help reduce the symptoms of COVID-19?
In terms of specifics: acetaminophen (Tylenol), naproxen (Aleve) or ibuprofen (Advil, Motrin) can help lower your fever, assuming you don’t have a health history that should prevent you from using them. It’s usually not necessary to lower a fever – an elevated temperature is meant to help your body fight off the virus.
Could deep breaths and forced coughs help treat COVID-19?
DEEP breaths and forced coughs could help clear mucus but are unlikely to help people with a dry cough and mild cases of covid-19, despite what advice on social media would have you believe. Breathing exercises help manage some respiratory conditions, like chronic obstructive pulmonary disease.
What is Continuous Positive Airway Pressure (CPAP) for COVID-19?
Continuous Positive Airway Pressure is a well-known device that is used for breathing assistant for the treatment of patients having a mild respiratory problem. The positive airway pressure is delivered through a tight face or nasal mask in CPAP device.

