In what format are health care claims sent
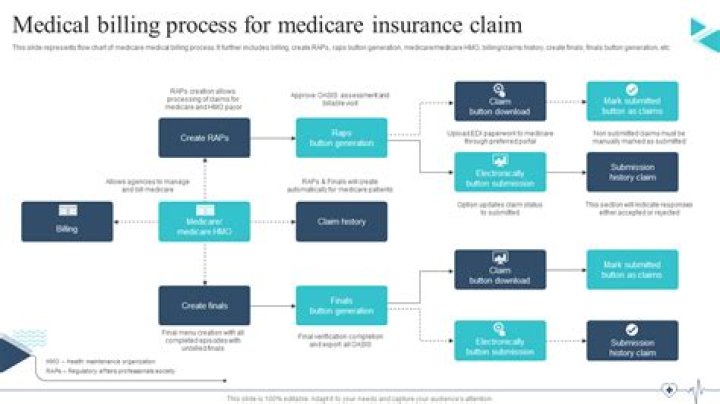
Most health care claims are submitted electronically, not on paper. Claim that is accepted by a health plan for adjudication. HIPAA-mandated electronic transaction for claims. The electronic HIPAA claim form, or the 837P claim, is based on the CMS-1500 claim, which is a paper claim form.
How are healthcare claims sent?
In most cases, claims are first transmitted to a clearinghouse. The clearinghouse reviews and reformats medical claims before sending them to the payer. In some cases, healthcare providers send medical claims directly to a payer. High-volume payers like Medicare or Medicaid may receive bills directly from providers.
What are 835 and 837 transactions?
The 837 files contain claim information and are sent by healthcare providers (doctors, hospitals, etc) to payors (health insurance companies). … The 835 files contain payment (remittance) information and are sent by the payors to the providers to provide information about the healthcare services being paid for.
What is the 837 file format?
An 837 file is an electronic file that contains patient claim information. This file is submitted to an insurance company or to a clearinghouse instead of printing and mailing a paper claim. The data in an 837 file is called a Transaction Set.What is an ANSI 837?
The 837 EDI document type is an electronic version of a paper Health Care Claim. Standard EDI formats include X12, ANSI, EDIFACT and its subsets. The 837 EDI document type is used to submit health care claim billing information, encounter information, or both, from health care service providers to payers.
What is medical claims submission process?
What Is Claim Submission? Submission of medical claims is one of the crucial steps in the medical billing process. The claim submission is defined as the process of determining the amount of reimbursement that the healthcare provider will receive after the insurance firm clears all the dues.
In what format are healthcare claims sent quizlet?
Most health care claims are submitted electronically, not on paper. Claim that is accepted by a health plan for adjudication. HIPAA-mandated electronic transaction for claims. The electronic HIPAA claim form, or the 837P claim, is based on the CMS-1500 claim, which is a paper claim form.
Which is an electronic format supported for healthcare claims transactions?
The transaction standard for health care claims or equivalent encounter data, professional, is the ASC X12N 837 format.What is the 835 file format?
ERA/835 Files The Electronic Remittance Advice (ERA), or 835, is the electronic transaction that provides claim payment information. These files are used by practices, facilities, and billing companies to auto-post claim payments into their systems.
What is the standard format used for submission of electronic claims for professional healthcare services?The 837 file is the standard format used by healthcare professionals and suppliers to transmit healthcare claims electronically in batch. One 837 file can contain thousands of claims, all submitted to the payer in one transaction.
Article first time published onWhat is a 270 271 file?
The 270 Transaction Set is used to transmit Health Care Eligibility Benefit Inquiries from health care providers, insurers, clearinghouses and other health care adjudication processors. … The 271 Transaction Set is the appropriate response mechanism for Health Care Eligibility Benefit Inquiries.
What is a 270 file?
The EDI 270 Health Care Eligibility/Benefit Inquiry transaction set is used to request information from a healthcare insurance plan about a policy’s coverages, typically in relation to a particular plan subscriber. … It may be used to inquire about general information on coverage and benefits.
How do I read an 835 file?
READING A PROFESSIONAL RA The ASC X12N 835 format is for electronic transfers only. Professional Providers can get free translator MREP software for viewing HIPAA 835 files from their MAC. You can either use the free MREP software or purchase other proprietary translator software.
What is ANSI format in medical billing?
American National Standard Institute (ANSI) codes are used to explain the adjudication of a claim and are the CMS approved. Group codes must be entered with all reason code(s) to establish financial liability for the amount of the adjustment or to identify a post-initial-adjudication adjustment.
What is ANSI 5010 format?
The 5010 HIPAA transaction standards are a new set of standards that regulate the electronic transmission of specific health care transactions. These include eligibility, claim status, referrals, claims and electronic remittance.
What are electronic claim forms?
An “electronic claim” is a paperless patient claim form generated by computer software that is transmitted electronically over telephone or computer connection to a health insurer or other third-party payer (payer) for processing and payment.
What is Hipaa EDI transactions?
Under the HIPAA EDI rule, a HIPAA electronic transaction is an electronic exchange of information between two parties to carry out financial or administrative activities related to healthcare. For example, a healthcare provider will send a claim to a health plan to request payment for medical services.
What is monitor payer adjudication?
Monitor Claim Adjudication Adjudication is the process by which payers evaluate medical claims and determine whether they are valid and compliant, and if so, the amount of reimbursement the provider will receive.
Which of the following is an electronic claim transaction the Hipaa health care claim or equivalent encounter information?
The HIPAA-mandated electronic transaction for claims is the HIPAA X12 837 Health Care Claim or Equivalent Encounter Information, and is usually called the “837 claim” or the “HIPAA claim.”
What is the first step in processing a claim?
- Claims Adjudication.
- Explanation of Benefits (EOBs)
- Claims Settlement.
What are claims in healthcare?
A request for payment that you or your health care provider submits to your health insurer when you get items or services you think are covered.
How are insurance claim forms usually prepared?
How are insurance claim forms usually prepared? The medical assistant prepares claims using a computer billing (EHR) or submits claim information to an insurance billing clearinghouse.
What is a 277 file?
The Claim Status Response (277) transaction is used to respond to a request inquiry about the status of a claim after it has been sent to a payer, whether submitted on paper or electronically. Once we return an acknowledgment that a claim has been accepted, it should be available for query as a claim status search.
What is an EDI 820?
An EDI 820 is a type of EDI transaction, which is used to transfer payment data between buyers and sellers. … Usually, an EDI 820 is sent jointly with the payment itself via electronic funds transfer.
Under what circumstances will a claim not be submitted electronically?
When phone or power services have been interrupted through no fault of the provider (e.g., by a storm or flood). When a provider or supplier submits fewer than 10 claims a month. When services are furnished only outside of U.S. territory.
Is EDI and Payer ID the same?
The Payer ID or EDI is a unique ID assigned to each insurance company. It allows provider and payer systems to talk to one another to verify eligibility, benefits and submit claims. … The payer ID is often located on the back of the insurance card in the Provider or Claims Submission section.
What is healthcare EDI for insurance claims processing?
Healthcare EDI provides secure electronic data interchange between healthcare institutions, care providers, and patients, and allows for more secure and efficient data processing, including healthcare claims processing.
Who uses CMS 1500 forms?
The CMS-1500 form is the standard claim form used by a non-institutional provider or supplier to bill Medicare carriers and durable medical equipment regional carriers (DMERCs) when a provider qualifies for a waiver from the Administrative Simplification Compliance Act (ASCA) requirement for electronic submission of …
What is UB 04 form used for?
An itemized medical bill lists in detail all the services that were provided during a visit or stay—such as a blood test or physical therapy—and may be sent to the patient directly. The UB-O4 form is used by institutions to bill Medicare or Medicaid and other insurance companies.
What is known as is the standard format used by health care professionals and suppliers to transmit health care claims electronically?
A company that often serves as the middleman between providers and billing groups, payers, and other health care partners for the transmission and translation of electronic claims information into the specific format required by payers is known as: … electronic claims tracking.
How does a 270 271 transaction work?
The 270 transaction is the EDI function that requests eligibility and benefit information from the Insurance Company of the patient. … The 271 transaction is the EDI function that responds eligibility and benefit information of the patient. It is set to receive care, from the Insurance Company to the Provider of Service.