What is a sacral decubitus ulcer
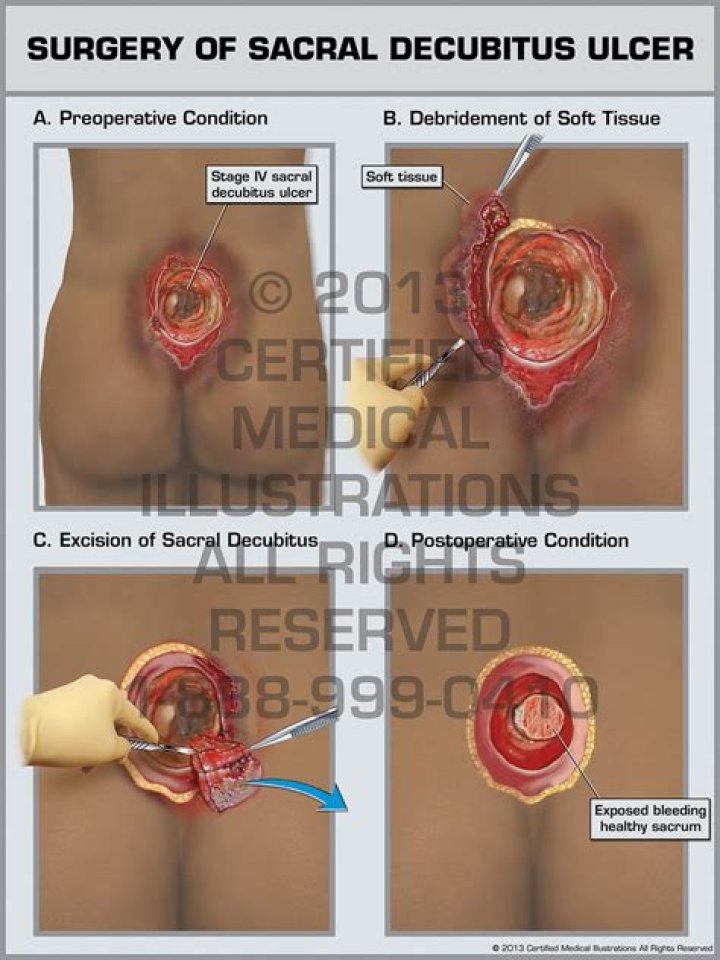
Decubitus ulcers are open wounds on the skin, usually found around bony areas of the body, including the sacral region. The sacral region is near the lower back at the bottom of the spine. Ulcers often form in people who are bedridden and are not able to move their bodies.
What causes sacral decubitus ulcer?
Prolonged pressure is essentially the main cause of a decubitus ulcer. Lying on a certain part of your body for long periods causes your skin to break down. The areas around the hips, heels, and tailbone are especially vulnerable to these types of sores.
What is sacral ulcer?
A sacral ulcer is a type of pressure injury (also called a decubitus ulcer or bedsore) caused by lengthy periods of direct pressure over a bony area of the body. The sacral region of the body lies between the L5 segment of the lumbar spine and the coccyx (tailbone).
How long does it take for a sacral ulcer to heal?
Pressure ulcers, also known as bedsores or decubitus ulcers, can take anywhere from three days to two years to heal.How do you treat a sacral wound?
Clean open sores with water or a saltwater (saline) solution each time the dressing is changed. Putting on a bandage. A bandage speeds healing by keeping the wound moist. It also creates a barrier against infection and keeps skin around it dry.
What does decubitus mean in medical terms?
Medical Definition of decubitus 1 : a position assumed in lying down the dorsal decubitus. 2a : ulcer. b : bedsore. 3 : prolonged lying down (as in bed)
Where is a sacral decubitus ulcer located?
Sacral decubitus ulcers are a certain type of wound located on the lower back at the bottom of the spine.
Can bed sores lead to death?
Stage 4 bedsores can lead to life-threatening infections. Bedsores cause over 60,000 deaths each year according to the Agency for Healthcare Research and Quality (AHRQ) and are often the tragic result of nursing home neglect.How do you treat decubitus?
- Removing pressure on the affected area.
- Protecting the wound with medicated gauze or other special dressings.
- Keeping the wound clean.
- Ensuring good nutrition.
- Removing the damaged, infected, or dead tissue (debridement)
- Transplanting healthy skin to the wound area (skin grafts)
Bedsores are wounds that form due to prolonged pressure on the skin. The fastest way to get rid of bedsores is to relieve the pressure, keep the wound clean, take antibiotics and to employ other strategies. Bedsores are wounds that develop over several days or months due to prolonged pressure on the skin.
Article first time published onHow is decubitus ulcer diagnosed?
Diagnosis of a Decubitus Ulcer Medical personnel may take samples of the pressure ulcer tissue and fluid to look for bacteria or cancer. They may also do blood cultures, bone scans or other tests depending on the seriousness of the ulcer.
How long does it take for a decubitus ulcer to develop?
Findings from the three models indicate that pressure ulcers in subdermal tissues under bony prominences very likely occur between the first hour and 4 to 6 hours after sustained loading.
What bacteria causes decubitus ulcers?
The most common organisms identified in pressure ulcers were Staphylococcus aureus, Proteus mirabilis, Pseudomonas aeruginosa, and Enterococcus faecalis.
Is zinc oxide good for bed sores?
Results showed that topical zinc oxide had increased wound healing, increased reepithelialization, decreased rates of infection and decreased rates of deterioration of ulcers. Topical zinc oxide has shown to improve the rate of wound healing in patients, regardless of their zinc status.
How do you treat an ulcer wound?
- Dressing. Dressings protect the wound and keep it clean. …
- Antibiotics. If your ulcer is infected, you’ll need antibiotic ointment. …
- Pain medication. At first, changing the dressing will be painful. …
- Surgery. Typically, noninfected skin ulcers don’t need surgery.
What is the pathophysiology of decubitus ulcers?
A decubitus ulcer is a wound that develops in the upper layers of the skin as the result of sustained, externally applied pressure and then enlarges both radially and into the deeper tissue layers.
How do pressure ulcers affect patients?
People with grade four pressure ulcers have a high risk of developing a life-threatening infection. The characteristics are: Full thickness skin loss with extensive destruction, tissue necrosis, or damage to muscle, bone, or supporting structures, for example, tendon or joint capsule.
What does purulent mean in medical terms?
Medical Definition of purulent 1 : containing, consisting of, or being pus a purulent discharge a purulent lesion.
What is the difference between recumbent and decubitus?
As nouns the difference between recumbent and decubitus is that recumbent is a bicycle or tricycle that places the rider in a reclined posture while decubitus is a bedsore.
What is the best cushion for bed sores?
- Gel Foam Wheelchair Cushion (14888) by Drive Medical. …
- Gel Supreme Wheelchair Cushion (KHPKBGSxxxx) by Gel Supreme. …
- Protekt O2 Cushion (LV7800X) by Proactive Medical. …
- Anti-Thrust Gel Foam Cushion for Geri Chair (75985300) by Skil-Care.
Are bedsores curable?
The sores are treatable, although full healing is not always possible. Without treatment, the sores can eventually lead to potentially fatal complications.
Why is it so common for patients to develop decubitus ulcers in long term care facilities?
In particular, long-term care residents are at high risk of developing pressure ulcers because of immobility,4 poor nutritional status,5 impaired mental status,6 and incontinence.
Are bed sores due to neglect?
However, bedsores can often be prevented with the right care plan in place. Their occurrence can be a sign of nursing home neglect. A variety of factors can contribute to the development of pressure ulcers, but they are overwhelmingly due to prolonged pressure on a certain area of the body.
How much is a bedsore lawsuit worth?
In cases where bedsores lead to infection and hospitalization, a bedsore lawsuit settlement may be in the region of $500,000 or more. In cases where patients have Stage 4 bedsores that lead to considerable pain, suffering and permanent long-term harm, the settlement range may be significantly higher than $500,000.
Is A and D ointment good for bed sores?
After cleaning, apply an ointment (such as A+D ointment) to keep the area dry. Use underpads to keep the patient from soiling the bed and to make it easier to clean up. Don’t use plastic underwear unless the patient is out of bed. If the skin has an open sore, ask about special dressings to help protect it.
What antibiotics are used for pressure ulcers?
Amoxicillin-potassium clavulanate is a naturally occurring beta-lactam structurally similar to the penicillin nucleus. This antibiotic group of beta-lactam/beta-lactamase combination has demonstrated a broad-spectrum activity; therefore, it is frequently used for the treatment of infected pressure ulcers.
How do you stage a sacral decubitus ulcer?
- Stage 1: The skin is red and irritated, but still intact. …
- Stage 2: The skin begins to break apart. …
- Stage 3: The tissue decay progresses past the first two layers of the skin. …
- Stage 4: The wound has reached all the way through the skin to muscle, bone, or tendons underneath.
Which of the following conditions would identify as risk factors for developing decubitus ulcers?
Risk Factors In addition to immobility and recuperation from surgery, other factors which may increase the risk of developing pressure ulcers include: poor nutrition, dehydration, diabetes, peripheral vascular disease, low albumin levels/anemia and obesity.
What do bedsores look like?
Bedsores occur in stages: Stage 1 has unbroken, but pink or ashen (in darker skin) discoloration with perhaps slight itch or tenderness. Stage 2 has red, swollen skin with a blister or open areas. Stage 3 has a crater-like ulcer extending deeper into the skin.
What areas are vulnerable to pressure ulcer damage?
Pressure injuries are usually caused by unrelieved pressure on the skin. They often form on skin that covers bony areas. The most common sites are the back of the head and ears, the shoulders, the elbows, the lower back and buttocks, the hips, the inner knees, and the heels.
Why don't you get bed sores when you sleep?
We normally move about constantly, even in our sleep. This stops pressure sores developing. People who are unable to move around tend to put pressure on the same areas of the body for a long time. If you are ill, bedridden or in a wheelchair, you are at risk of getting pressure sores.