What is cytarabine syndrome
Cytarabine syndrome is a rare clinical condition characterized by fever, malaise, myalgia, arthralgia, and/or rash that occurs after receipt of cytarabine. Our patient developed fever, malaise, and diffuse body pain shortly following cytarabine initiation despite receiving prophylactic dexamethasone.
Which conditions are symptoms of cytarabine syndrome?
The Cytarabine (Ara-C) Syndrome It is characterized by fever, myalgia, bone pain, occasionally chest pain, maculopapular rash, conjunctivitis and malaise. It usually occurs 6 to 12 hours following drug administration. Corticosteroids have been shown to be beneficial in treating or preventing this syndrome.
What are the side effects of cytarabine Ara C and idarubicin?
- Hair loss (nearly all patients will lose their hair temporarily)
- Mouth ulcers [mucositis] (15%)
- Neutropenic fever (8 – 29%)
- Nausea or vomiting (exact % is unknown)
- Decreased appetite (exact % is unknown)
- Bleeding (1%)
How do you treat cytarabine rash?
Though its appearance is aggressive there are no other associated symptoms. The rash resolves without subsequent sequelae. Treatment includes application of emollients and triamcinolone. Cytarabine therapy should not be terminated due to this rash.What is cytarabine used for?
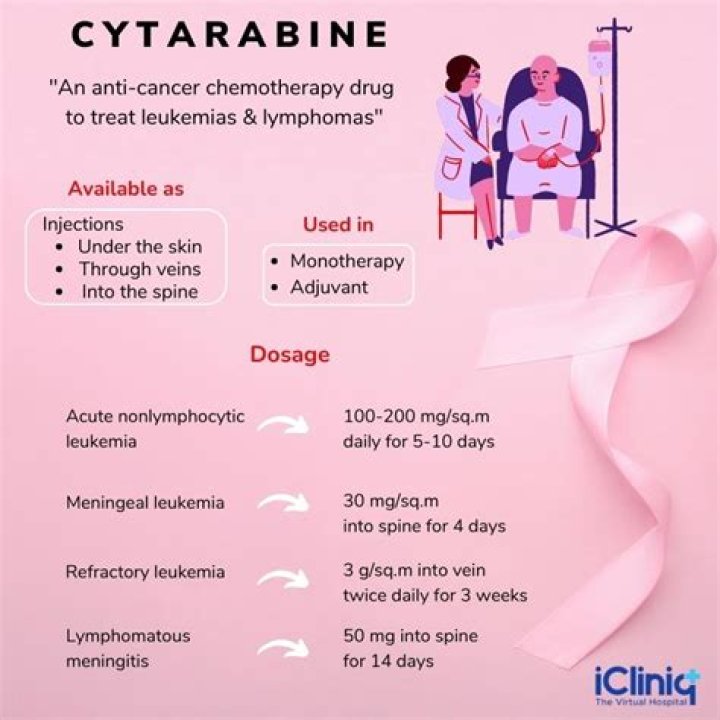
Cytarabine is used alone or with other chemotherapy drugs to treat certain types of leukemia (cancer of the white blood cells), including acute myeloid leukemia (AML), acute lymphocytic leukemia (ALL), and chronic myelogenous leukemia (CML).
How long does Cytarabine stay in your body?
Nadir: White blood cells: 7-10 days, platelets: 12-15 days.
How is Cytarabine cleared?
It has an active metabolite- azacytidine triphosphate; and an inactive metabolite- uracil arabinoside, which is cleared by the kidney.
Where does cytarabine come from?
The isolation of C-nucleosides from the Caribbean sponge, Cryptotheca crypta, four decades ago, provided the basis for the synthesis of cytarabine, the first marine-derived anticancer agent to be developed for clinical use. Cytarabine is currently used in the routine treatment of patients with leukaemia and lymphoma.How does cytarabine affect the skin?
Skin changes Cytarabine can cause a rash, which may be itchy. It may also cause your skin to become red or blistered. Always tell your doctor or nurse about any skin changes. They can give you advice and may prescribe creams or medicines to help.
Does cytarabine cause hair loss?This medicine may cause a temporary loss of hair in some people. After treatment with cytarabine has ended, normal hair growth should return.
Article first time published onHow many rounds of chemo is needed for leukemia?
Most people have 2 rounds of induction chemotherapy. The treatment will be carried out in hospital or in a specialist centre, as you’ll need very close medical and nursing supervision. You may be able to go home between treatment rounds.
What is the survival rate of AML?
The 5-year survival rate for people 20 and older with AML is 26%. For people younger than 20, the survival rate is 68%. However, survival depends on several factors, including biologic features of the disease and, in particular, a patient’s age (see Subtypes for more information).
Can Cytarabine cause neuropathy?
Intravenous (IV) therapy may cause a peripheral neuropathy that varies greatly in its severity. The high IV cytarabine doses now commonly used can cause seizures, cerebral dysfunction, or an acute cerebellar syndrome with an incidence up to 14%.
Is cytarabine a chemo drug?
Cytarabine is a type of chemotherapy drug and is also known by its brand name, Ara C. It is a treatment for: acute leukaemias (cancers of the blood)
What is the strongest chemo drug?
Doxorubicin (Adriamycin) is one of the most powerful chemotherapy drugs ever invented. It can kill cancer cells at every point in their life cycle, and it’s used to treat a wide variety of cancers.
What are the side effects of cladribine?
- fever;
- nausea, vomiting, diarrhea;
- headache, tiredness;
- rash;
- cough; or.
- pain, bruising, swelling, or irritation where the medicine was injected.
How toxic is cytarabine?
The main toxic effect of cytarabine injection is bone marrow suppression with leukopenia, thrombocytopenia and anemia. Less serious toxicity includes nausea, vomiting, diarrhea and abdominal pain, oral ulceration, and hepatic dysfunction.
Which phase of the cell is most affected by cytarabine?
Its mode of action is due to its rapid conversion into cytosine arabinoside triphosphate, which damages DNA when the cell cycle holds in the S phase (synthesis of DNA). Rapidly dividing cells, which require DNA replication for mitosis, are therefore most affected.
How often is cytarabine given?
Intermittent dosing: Cytarabine may be given as intermittent intravenous doses of 3-5 mg/kg daily, for five consecutive days. This course of treatment can be repeated after an interval of 2 to 9 days and repeated until the therapeutic response or toxicity is exhibited.
How can I flush chemo out of my system?
Chemotherapy can be dehydrating. Drinking plenty of water before and after treatment helps your body process chemotherapy drugs and flush the excess out of your system.
Why do you have to flush the toilet twice after chemo?
Small amounts of chemotherapy are present in your body fluids and body waste. If any part of your body is exposed to any body fluids or wastes, wash the exposed area with soap and water. People in your household may use the same toilet as you, as long as you flush all waste down the toilet twice with the lid down.
Can cytarabine be given at home?
Cytarabine by subcutaneous injection is not given as frequently as intravenous but is a route of administration of Cytarabine in the home environment.
What is the best food to eat after chemo?
- Apple and grape juice.
- Fruit nectars.
- Low-salt broth.
- Clear soups.
- Gatorade.
- Popsicles and sherbert.
- Gelatin.
- Herbal teas, such as ginger and mint.
Which phase is affected by cytarabine?
Cytarabine is cytotoxic to a wide variety of proliferating mammalian cells in culture. It exhibits cell phase specificity, primarily killing cells undergoing DNA synthesis (S-phase) and under certain conditions blocking the progression of cells from the G1 phase to the S-phase.
Can you kiss a chemo patient?
Kissing is a wonderful way to maintain closeness with those you love and is usually okay. However, during chemotherapy and for a short time afterward, avoid open-mouth kissing where saliva is exchanged because your saliva may contain chemotherapy drugs.
What is the side effect of daunorubicin?
Cerubidine (daunorubicin) is a cancer (antineoplastic) medication used in the treatment of leukemia (blood cancer). Cerubidine is available in generic form. Common side effects of Cerubidine include nausea, vomiting, constipation, diarrhea, and loss of appetite. Cerubidine may cause urine to turn a reddish color.
Is cytarabine an immunosuppressant?
Used mainly in the treatment of leukaemia, especially acute non-lymphoblastic leukaemia, cytarabine is an antimetabolite antineoplastic agent that inhibits the synthesis of DNA. It also has antiviral and immunosuppressant properties.
How many rounds of chemo can a person have?
During a course of treatment, you usually have around 4 to 8 cycles of treatment. A cycle is the time between one round of treatment until the start of the next. After each round of treatment you have a break, to allow your body to recover.
How do I know if the chemo is working?
The best way to tell if chemotherapy is working for your cancer is through follow-up testing with your doctor. Throughout your treatment, an oncologist will conduct regular visits, and blood and imaging tests to detect cancer cells and whether they’ve grown or shrunk.
How effective is cytarabine?
The overall survival data with the use of cytarabine in conventional and high dose regimen is approximately 40% with remission rates of 70–80% and relapse-free 5 years survival of 40-70%[15]. Standard intensive treatment improves early death rates and long-term survival compared with palliation.
Which type of leukemia is most fatal?
Patients with the most lethal form of acute myeloid leukemia (AML) – based on genetic profiles of their cancers – typically survive for only four to six months after diagnosis, even with aggressive chemotherapy.

