What is dialyzer clearance
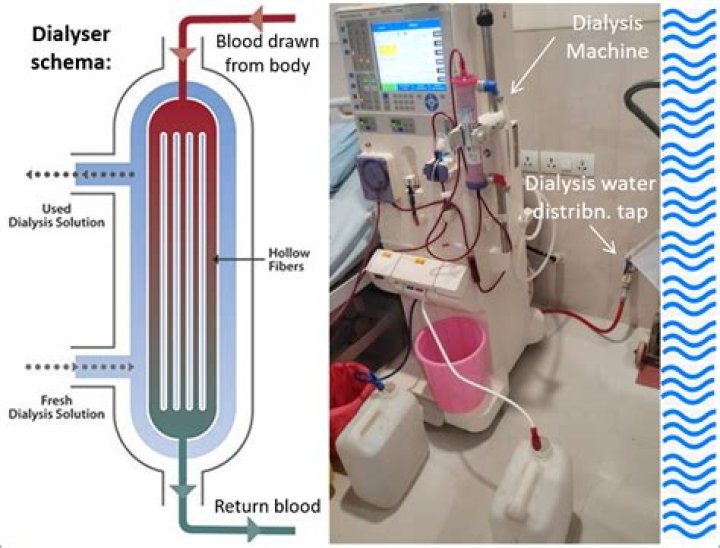
K stands for the dialyzer clearance, the rate at which blood passes through the dialyzer, expressed in milliliters per minute (mL/min) t stands for time. Kt, the top part of the fraction, is clearance multiplied by time, representing the volume of fluid completely cleared of urea during a single treatment.
What affects dialyzer clearance?
Blood flow, dialysate flow and surface area are the main determinants of the performance of a dialyzer, however the impact of each parameter on small and middle molecule clearance in high flux dialysis has not been well explored.
What is the difference between dialysis and dialyzer?
Hemodialysis and peritoneal dialysis are different ways to filter the blood. Dialysis is a procedure that helps your blood get filtered by a machine that works like an artificial kidney. Hemodialysis: Your entire blood is circulated outside your body in a machine placed outside the body known as a dialyzer.
What is solute clearance in hemodialysis?
Solute clearance is an objective means of quantifying the delivered dose of PD. There has been an evolution of clinical guidelines on the target dose of PD based on the solute clearance to ensure the provision of adequate dialysis for optimal patient survival.What is a Dialyser why is it used?
A dialyzer is often referred to as an “artificial kidney.” Its function is to remove the excess wastes and fluid from the blood, when the patient’s kidneys can no longer perform that task. Dialyzers are made of a thin, fibrous material.
What is removed during dialysis?
In hemodialysis, fluid is removed by ultrafiltration using the dialysis membrane. The pressure on the dialysate side is lower so water moves from the blood (place of higher pressure) to the dialysate (place of lower pressure). This is how the hemodialysis treatment removes fluid.
Does dialysis remove creatinine?
Dialysis removes fluid and wastes Waste such as nitrogen and creatinine build up in the bloodstream. If you have been diagnosed with CKD, your doctor will have these levels carefully monitored. One of the best indicators of kidney function is your glomerular filtration rate (GFR).
Why is reverse filtration important in dialysis?
The reverse osmosis (RO) system uses a pump to push water through a semipermeable membrane or filter which removes almost all of the contaminants including bacteria and viruses.What is solute clearance?
As noted above, solute clearance is the ratio of mass removal rate to blood solute concentration. From a kinetic perspective, Fig. 2 depicts the relevant flows for determining CRRT clearances. In CRRT, the solute clearance expressions differ from those used in conventional hemodialysis.
What is ultrafiltration coefficient?The ultrafiltration coefficient (KUF) is the permeability of a membrane to water per unit of pressure and surface area. A typical filter will have a KUF between 10-25 ml/h/mmHg/m2.
Article first time published onWhat are the 3 types of dialysis?
There are 3 main types of dialysis: in-center hemodialysis, home hemodialysis, and peritoneal dialysis. Each type has pros and cons. It’s important to remember that even once you choose a type of dialysis, you always have the option to change, so you don’t have to feel “locked in” to any one type of dialysis.
Which type of dialysis is best?
Peritoneal dialysis is an effective form of dialysis, has been proven to be as good as hemodialysis. Peritoneal dialysis is not for everyone. People must receive training and be able to perform correctly each of the steps of the treatment.
Which type of dialysis uses a dialyzer to filter the patient's blood?
Hemodialysis is a procedure where a dialysis machine and a special filter called an artificial kidney, or a dialyzer, are used to clean your blood. To get your blood into the dialyzer, the doctor needs to make an access, or entrance, into your blood vessels.
What are the types of dialyzer?
In addition, dialyzers are internationally classified into three types: low-flux, high-flux, and protein-leaking.
Can you reuse dialyzer?
There is no set number of times that is considered safe for dialyzer reuse. As long as the TCV test shows that the dialyzer is working well, and the dialyzer looks clean, it should be safe for you to reuse your dialyzer. Ask your dialysis care team if they have tested your dialyzer and if it still works well.
Why is my creatinine high after dialysis?
After a hemodialysis session, creatinine concentration reaches a nadir following equilibration between blood, extravascular and tissue fluid stores. Creatinine then starts to increase due to new generation and minimal renal clearance, reaching its peak before the next hemodialysis session.
Can kidneys start working again after dialysis?
The good news is that acute kidney failure can often be reversed. The kidneys usually start working again within several weeks to months after the underlying cause has been treated. Dialysis is needed until then.
What is normal creatinine level after dialysis?
The mean creatinine and BUN levels after cessation of dialysis were 2.85 ± 0.57 mg/dl and 29.62 ± 5.26 mg/dl, respectively, while the mean creatinine clearance calculated by 24-hour urine collection was 29.75 ± 4.78 ml/min.
What is isolated UF in hemodialysis?
Isolated ultrafiltration (removal of plasma water and solute without dialysis) was used as a “last resort” therapy in three patients with diuretic and pressor resistant oliguria complicating severe volume overload and vascular shock.
Can dialysis remove water from lungs?
Hemodialysis can remove the excess fluid from the body in overhydrated patients, which in turn reduces water content of the lungs and thus decreases the pressure on airways, and reduces obstruction [27].
What is the normal amount of fluid removed during dialysis?
Ideally, fluid removal rates should be less than 7-8 ml for every kg of body weight in each hour of dialysis.
How you will increase solute clearance during dialysis?
- Increasing the dialysate flow rate.
- Increasing the ultrafiltration rate.
- Increasing the replacement fluid rate.
How do I increase my peritoneal dialysis clearance?
It can be augmented by using large instillation volumes, by the application of more exchanges, and by increasing peritoneal ultrafiltration.
What is diffusion hemodialysis?
Summary of diffusion with hemodialysis The formal definition of diffusion in dialysis is movement of solutes as a result of random molecular motions across a semipermeable membrane down its concentration gradient. With dialysis most of the toxin removal is accomplished by diffusion.
What is a RO water system?
Reverse Osmosis (RO) is a water treatment process that removes contaminants from water by using pressure to force water molecules through a semipermeable membrane. During this process, the contaminants are filtered out and flushed away, leaving clean, delicious drinking water.
How do you clean a dialysis machine?
Routine Disinfection of the Dialysis Station ☐ Clean dialysis machine from top to bottom. If visible contaminant on the machine, wipe off using an absorbent material. Clean the machine using wipes/cloths with a disinfectant that is acceptable to the HD machine manufacturer and the HA renal program/infection control.
What is the primary device for purifying the water used in dialysis?
The most common method used to purify water for hemodialysis treatment is reverse osmosis. (Figure 2, Table 4). The reverse osmosis device is a self-contained unit that uses a high-pressure pump and a semipermeable membrane to purify water (Figure 2, Table 4).
What is TMP in ultrafiltration?
Transmembrane Pressure: The average applied pressure from the feed to the filtrate side of the membrane. TMP [bar] = [(PF + PR)/2] – Pf. For additional information, see Protein Concentration and Diafiltration by Tangential Flow Filtration — An Overview.
What is low flux dialyzer?
Low flux dialyzers are an option for acute and chronic dialysis where a lower rate of fluid removal (e.g., ultrafiltration coefficient) is desired. Explore our wide range of biocompatible, polysulfone dialyzers designed to meet the clinical needs of all patient types.
What is a buffer in dialysis?
Abstract. A buffer is included in the peritoneal dialysis solution in order to offset the hydrogen ions normally produced during the metabolic processes. Nowadays, the buffer used is lactate, and its concentration in conventional peritoneal dialysis fluids is 35 or 40 mmol/L.
What is soft dialysis?
The soft tube is called an access because it provides a way to get the dialysis liquid into your belly. The soft tube is usually placed in the operating room or a procedure room. It takes about two weeks for the skin to heal around the tube before dialysis can be started.