What is the difference between probationary period and elimination period
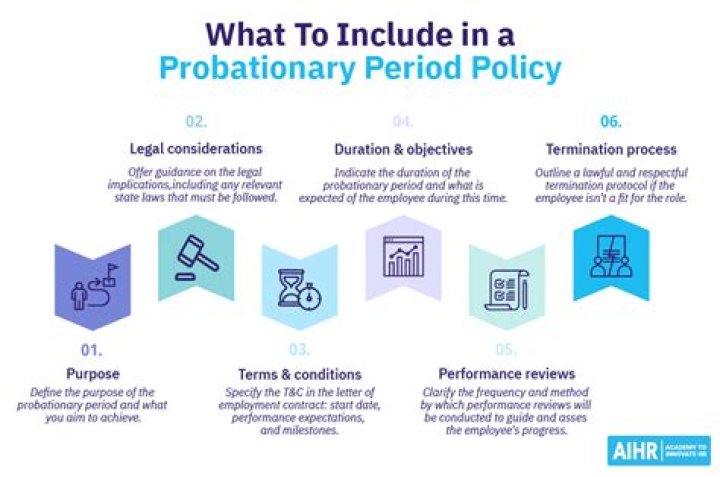
The probationary period is any time between when you fill in your application and you’re able to make a claim on your policy. The elimination period, seen most often in long-term disability policies, is the insurance waiting period between when you make your claim and when your first check is issued.
What does it mean elimination period?
Elimination period is a term used in insurance to refer to the time period between an injury and the receipt of benefit payments. In other words, it is the length of time between the beginning of an injury or illness and receiving benefit payments from an insurer.
Do you get paid during elimination period?
An elimination period works as follows. The elimination period is based on calendar days. No benefits are paid during the elimination period.
Is elimination period same as waiting period?
The elimination period is the time between the date of your injury or illness and the date you’re eligible to start receiving benefits. It’s a time-based deductible. The waiting period is the same regardless of when you file your disability claim, though it’s always best to file your claim as soon as possible.What does elimination period mean for short term disability?
Elimination Period: The elimination period is a period of time an employee must be disabled before benefits are paid. For short term disability, there is an elimination period for disabilities due to sickness and one for those due to injury.
How does elimination period work for long term care insurance?
An elimination period: Is like the deductible you have on car insurance, except it is measured in time rather than by dollar amount. Most policies allow you to choose an elimination period of 30, 60, or 90 days at the time you purchased your policy. During the period, you must cover the cost of any services you receive.
What is a probationary period in insurance?
The waiting – or probationary – period is the period of time set by an employer before coverage becomes effective for a new employee enrolling into the group’s health benefit coverage. Group health plans and health insurance carriers that offer group coverage may not apply a probationary period that exceeds 90 days.
What does a probationary period provision establish?
Probationary Period — a provision in some disability income policies stipulating that benefits will not be payable for sickness commencing during a specified time period (e.g., 15–30 days) after inception of the policy.What is a 14 day elimination period?
The Elimination Period means “the period of your disability during which MetLife does not pay benefits.” The Elimination Period starts on the day you become disabled and continues for the period shown in your Schedule of Benefits. … Option A has an Elimination Period of 14 days for both accident and sickness.
What is the difference between FMLA and short term disability?Short-term disability insurance generally replaces about 60% of your income from three months to one year (sometimes longer). FMLA protects your job for 12 weeks while you are on medical leave, but it does not provide pay. … Disability insurance may also pay benefits after your FMLA leave expires.
Article first time published onWhich of the following is a primary purpose of the elimination period which appears in a long term disability policy?
The purpose of the elimination period is to prevent the insurer from paying short-term disabilities. … Her disability income policy will not pay benefits because her injury was not unforeseen.
Does a 90 day elimination period for LTD insurance raise the cost of the policy?
The typical elimination period is 90 days. You can alter the cost of your policy by changing its elimination period. Longer elimination periods provide cheaper premiums; policies with shorter elimination periods have higher premiums.
Which of the following is true regarding the elimination periods and the cost of coverage?
Which of the following is true regarding elimination periods and cost of coverage? The longer the elimination period, the lower the cost of coverage. – the elimination period is a period of days which must expire after onset of an illness or occurrence of an accident before benefits will be payable.
What is the main difference between coinsurance and copayments?
A copay is a set rate you pay for prescriptions, doctor visits, and other types of care. Coinsurance is the percentage of costs you pay after you’ve met your deductible.
What is a common elimination period for care received at home?
Elimination Periods: The most common options are 0 days, 30 days, 90 days or 100 days. Some policies only make you meet the Elimination Period once during the life of the policy; others apply it again after you have gone for a certain period of time without needing care.
What is the shortest possible elimination period for group?
What is the shortest possible elimination period for group short-term disability benefits provided by an employer? 0 days; If an employer provides short-term disability benefits for its employees, the elimination period can be nonexistent, and the benefits can last as long as two years.
How does an elimination period work in disability income policies?
The Elimination Period is defined as the period starting from the day you first become disabled and continuing for the period noted in the policy. This may be 90 days or 180 days or whatever the policy calls for. No Benefits Paid: During the EP, no benefits are paid.
What is another term for probationary period?
Noun. A period in which one is undergoing a trial. probation. training. traineeship.
Is a probationary period normal?
LENGTH OF PROBATIONARY PERIOD There is no law determining the length of a probationary period. However, there is an expectation that the employer will be reasonable. It is typical for a probationary period to last no longer than six months, and three months where an employee is moving to a new post internally.
Is a probationary period mandatory?
Legally, there’s no such thing as a probationary period. Once you’ve started work, the number of weeks you’ve worked begins on the day you started, not from the time when your probationary period ended. Your full contractual rights also started from your first day of work, unless your contract says otherwise.
What qualifies as short-term disability?
To qualify for short-term disability benefits, an employee must be unable to do their job, as deemed by a medical professional. Medical conditions that prevent an employee from working for several weeks to months, such as pregnancy, surgery rehabilitation, or severe illness, can qualify to receive benefits.
Is paid family leave the same as short-term disability?
Paid family leave is also known as “family caregiver leave” or “family leave insurance.” Paid medical leave is also known as “temporary disability insurance” (TDI) or “short-term disability.” Paid family and medical leave together are also referred to as “family and medical leave insurance” (FMLI).
Do you accrue PTO while on short-term disability?
Employees on unpaid leave are not entitled to continue accruing paid-leave benefits. This includes employees who are receiving income replacement benefits from a source other than [Company Name] payroll such as short-term disability, long-term disability or workers’ compensation insurance.
What is 0 day elimination period?
Zero-Day Home Care Elimination Period = A feature in a long-term care insurance policy that waives the elimination period for qualified care received at home. The policy can pay benefits for the first day of qualified care received at home.
Do you have to pay back long term disability?
A person who is also receiving LTD benefits will generally be expected to pay back the insurance company from this pay out from SSDI. … You received a past-due lump sum payment in the amount of $10,000, which covers each month from the date of your initial disability (per the SSA) until the current month.
What is STD insurance?
Short-term disability insurance (STD) provides a source of income should you experience a short-term illness or injury that prevents you from working. Long-term disability insurance (LTD) provides a source of income should you experience a long-term illness or injury that prevents you from working.
What is the best waiting period for disability insurance?
A 90-day elimination period is usually the best way to get the protection you need while keeping your disability insurance policy affordable.
What are the benefits of long term disability?
Long-term disability insurance helps ensure that employees will still receive a portion of their income when they are absent from work for an extended period due to a covered disability. These absences may be a result of accidents, injuries or illnesses that happened on or off the job.
What is the main difference between coinsurance and copayments quizlet?
copay is the amount you will pay overtime you use medical services. coinsurance is the percentage each party pays for medical services. max out of pocket is the maximum limit you must pay for that period. You just studied 7 terms!
What is the difference between PPO and HDHP?
A high deductible plan is a type of health insurance with higher deductibles but lower premiums. … A preferred provider organization (PPO) is a plan type with lower deductibles but higher monthly premiums.
What's HMO and PPO mean?
HMO stands for health maintenance organization. POS stands for point of service. PPO stands for preferred provider organization.