What is the difference between PRVC and Simv
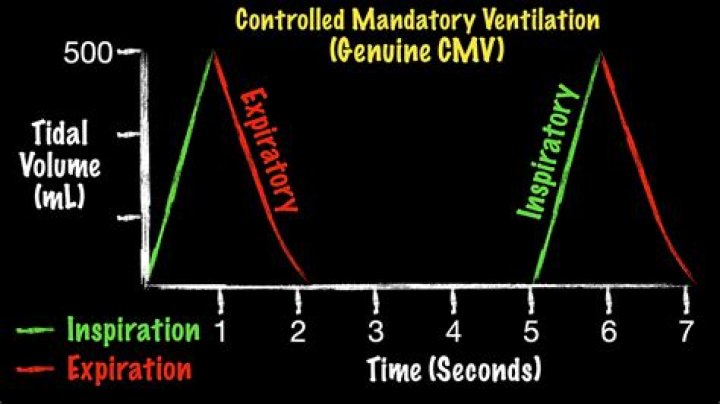
The PRVC mode is better than the volume controlled SIMV mode in ventilating COPD patients with acute exacerbations and type II respiratory failure. The PRVC mode showed faster improvement, shorter ICU stay, fewer complications and lower peak inspiratory airway pressures.
What is Simv PRVC mode?
SIMV: PRVC+PS. PC (Pressure Controlled Ventilation) servo i. In this controlled mode of ventilation, the ventilator delivers a breath to a set pressure, and at a set rate. This is primarily used when the patient has no spontaneous breathing but will support the patient if they are able to trigger a breath.
What is PRVC vent setting?
Pressure-regulated volume control (PRVC) is a mode of ventilation in which the ventilator attempts to achieve set tidal volume at lowest possible airway pressure. This mode of ventilation is being commonly used as the initial mode of ventilation in many intensive care units.
When should I use PRVC mode?
It is considered a dual mode of ventilation that uses a decelerating waveform. PRVC is an appropriate mode of ventilation for patients who require a specific tidal volume (VT) with the lowest effective pressure, such as those with acute respiratory distress syndrome (ARDS).What are the 4 methods of full ventilatory support?
These are: Assist/Control ventilation (A/C), Pressure Support Ventilation (PSV) and Synchronized Intermittent Mandatory Ventilation (SIMV) with PS, a hybrid mode of the first two.
Why is SIMV used in pediatrics?
Pediatric patients are more likely than their adult counterparts to over-breathe the set respiratory rate, putting them at risk of breath stacking from large volume breaths. SIMV can help to mitigate this risk [2].
Is VC plus the same as PRVC?
Other pressure modes include pressure support ventilation (PSV), pressure-regulated volume control (PRVC, also known as volume control plus [VC+]), airway pressure release ventilation (APRV), and biphasic ventilation (also known as BiLevel).
What does VC+ mean?
VC + ventilation (Volume control. plus ventilation) • VC+ ventilation is an alternative method of ventilation. used to ventilate patients with ARDS.When do you use Avaps in non invasive ventilation?
AVAPS is a safe strategy of noninvasive ventilatory treatment in patients with exacerbations of COPD and hypercapnic encephalopathy (GCS < 10).
Is CPAP a ventilator?CPAP is Continuous Positive Airway Pressure. It is a type of non-invasive ventilation (NIV) or breathing support.
Article first time published onWhat is spontaneous mode of ventilation?
Continuous spontaneous ventilation is any mode of mechanical ventilation where every breath is spontaneous (i.e., patient triggered and patient cycled). Spontaneous breathing is defined as the movement of gas in and out of the lungs that is produced in response to an individual’s respiratory muscles.
What is the full form of PRVC?
Pressure-regulated volume control (PRVC) is a new mode of ventilation that combines the advantages of the decelerating inspiratory flow pattern of a pressure-control mode with the ease of use of a volume-control (VC) mode.
Is CPAP with pressure support the same as BiPAP?
BiPAP offers the same support as CPAP with the added ability to further decrease work of breathing during exhalation and improve tidal volumes thereby clearing more CO2 than CPAP.
What is the difference between CPAP and PSV?
In both groups, PSV showed lower end tidal carbon dioxide (P < 0.001), higher oxygen saturation, (P < 0.001), and higher expired tidal volume (P < 0.001) compared with CPAP. In both groups, PSV had similar leak fraction, respiratory rate, mean arterial pressure, and heart rate compared with CPAP.
What are the two types of medical ventilation?
- Positive-pressure ventilation: pushes the air into the lungs.
- Negative-pressure ventilation: sucks the air into the lungs by making the chest expand and contract.
Is SIMV the same as BiPAP?
The main differences between SIMV and BiPAP are that SIMV does not allow spontaneous breathing during the mandatory breaths, whereas spontaneous breathing is possible during all phases with BiPAP, and that with SIMV, all mandatory breaths are volume- or pressure-targeted, whereas BiPAP provides only pressure-targeted …
Why is SIMV bad?
Now, Robinson et al identify another disadvantage of SIMV: that it is associated with ventilator asynchrony. Although there were no other adverse clinical outcomes associated with its use, these could certainly occur in a sicker less stable patient population.
What may cause ventilator patient asynchrony in premature infants?
End inspiratory asynchrony occurs because of delayed triggering or excessively long ventilator breaths. Reports indicate that most mechanical breaths extend beyond the end of the preterm infant’s spontaneous inspiration.
Is Avaps better than Bipap?
Although both AVAPS and BiPAP are reliable in the treatment of acute hypercapnic respiratory failure, AVAPS is associated with a speedy improvement of the patient clinically. The patients have also experienced greater comfort and satisfaction comparatively, and therefore, improved treatment-compliance.
Is Avaps a Bipap?
Bilevel positive airway pressure-spontaneous/timed (BiPAP S/T) with average volume assured pressure support (AVAPS) uses a fixed tidal volume that automatically adjusts to a patient’s needs.
What is the difference between Avaps and Avaps AE?
In AVAPS, if the targeted tidal volume is not reached, the ventilator takes over to provide necessary pressure support to reach the goal [2]. In AVAPS-AE, the ventilator automatically increases the defined pressure support to reach the target tidal volume together with increasing EPAP.
What is VC+ Plus on ventilators?
The Puritan Bennett™ Volume Ventilation Plus software option combines the benefits of pressure and volume ventilation using Volume Control Plus and Volume Support modes. In Volume Control Plus, clinicians set the inspiratory time and desired tidal volume. In Volume Support, clinicians set the desired tidal volume.
What is AC VC?
VC/AC – Volume Control/Assist Control – the ventilator is set to deliver a specific volume each breath, regardless of the amount of pressure required to deliver the volume.
What is volume control ventilation?
Volume Control Ventilation (VCV), has been the traditional controlled ventilation mode in anesthesia. In VCV, the ventilator delivers the preset tidal volume (TV) with a constant flow during the preset inspiratory time (Ti) at the preset respiratory rate.
Can CPAP damage your lungs?
There is no indication that CPAP can damage your lungs. Some people report a burning sensation in their lungs following CPAP use. However, this is usually the result of inhaling cold, dry air.
Does CPAP push fluid out of the lungs?
The CPAP device often prevents the need for a breathing tube because oxygen can be given through the breathing mask to push the fluid out of the lungs and back into the bloodstream where it belongs. The relief is almost immediate, says James McCarthy, medical director at Memorial Hermann s emergency center.
What is the difference between ventilator and respirator?
Your doctor might call it a “mechanical ventilator.” People also often refer to it as a “breathing machine” or “respirator.” Technically, a respirator is a mask that medical workers wear when they care for someone with a contagious illness. A ventilator is a bedside machine with tubes that connect to your airways.
What is the most common ventilator mode?
Mechanical ventilation is a lifesaving procedure that is often performed when patients require respiratory support. [1] Assist-control (AC) mode is one of the most common methods of mechanical ventilation in the intensive care unit[2]. AC ventilation is a volume-cycled mode of ventilation.
What does C mean on ventilator?
ASSIST CONTROL (AC) OR CONTINUOUS MANDATORY VENTILATION (CMV) Assist Control (or “AC”) is a term used to describe the number of breaths a patient is receiving from the breathing machine (ventilator). AC refers to a specific method for giving the patient mechanical breaths.
What are the different ventilator modes?
VariablePressure support breathLimiting/controlPressure
Is PRVC good for ARDS?
Conclusions: Although it is not possible to draw any conclusion on morbidity and mortality in patients treated with PRVC versus VC, for gas exchange and compliance improvement and for inspiratory pressure decrease with consequent reduction of barotrauma, it may be affirm that PCRV seems to be the best ventilation …