What lab results would likely be seen in a person who is diagnosed with osteomalacia
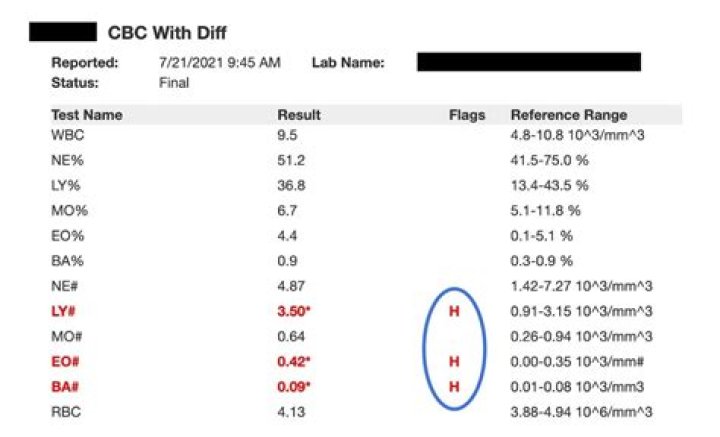
Your healthcare provider may also test you for alkaline phosphatase isoenzymes. High levels indicate osteomalacia. Another blood test can check your levels of parathyroid hormone. High levels of this hormone suggest insufficient vitamin D and other related problems.
What are the key lab features in osteomalacia?
Major typical biochemical findings include: Low serum and urinary calcium. Low serum phosphate, except in cases of renal osteodystrophy. Elevated serum alkaline phosphatase (due to an increase in compensatory osteoblast activity)
Does hypercalcemia cause osteomalacia?
Patients with multiple myeloma may also have anemia and decreased renal function. Primary hyperparathyroidism should present with hypophosphatemia, increased bone alkaline phosphatase, and increased zones of uptake. However, it usually presents with hypercalcemia, which is atypical in osteomalacia.
Which diagnostic test may be used to confirm a diagnosis of osteomalacia?
Diagnosis and Tests X-rays may be taken to see if there is any evidence of osteomalacia. A bone mineral density scan may be helpful in evaluating the amount of calcium and other minerals present in a patient’s bone segment.Why is alkaline phosphatase high in osteomalacia?
Increased serum alkaline phosphatase or bone specific alkaline phosphatase activity is classically associated with osteomalacia due to vitamin D deficiency but is not an early or reliable clue because some patients may have normal or only borderline elevated levels.
What body system does osteomalacia affect?
Osteomalacia causes the bones to become soft, which can lead to pain and bone deformity. Bones need calcium and phosphate to stay strong, and without the proper levels of vitamin D in the body, bones are unable to absorb enough calcium and phosphate minerals to remain healthy.
What lab tests are used to diagnose osteoporosis?
Dual-energy x-ray absorptiometry (DXA) is the gold standard test for diagnosis. Laboratory testing is useful in ruling out secondary causes of osteoporosis.
What causes osteomalacia in adults?
Vitamin D deficiency. People who live in areas where sunlight is limited, get little exposure to sunlight or eat a diet low in vitamin D can develop osteomalacia. Vitamin D deficiency is the most common cause of osteomalacia worldwide.Can a bone density test show osteomalacia?
Based on our investigation, low BMD in amount of osteoporosis results by bone densitometry may be detected in up to 70% of patients with osteomalacia.
What is the difference between osteopenia and osteomalacia?Osteopenia is decreased bone mass. Two metabolic bone diseases decrease bone mass: osteoporosis and osteomalacia. In osteoporosis, bone mass decreases, but the ratio of bone mineral to bone matrix is normal. In osteomalacia, the ratio of bone mineral to bone matrix is low.
Article first time published onCan blood tests detect osteoporosis?
Blood tests are another method used to diagnose certain bone diseases. One example is osteoporosis, where blood tests are used to determine risk factors and rule out other illnesses.
What is the most common assessment finding associated with osteoporosis?
To diagnose osteoporosis and assess your risk of fracture and determine your need for treatment, your doctor will most likely order a bone density scan. This exam is used to measure bone mineral density (BMD). It is most commonly performed using dual-energy x-ray absorptiometry (DXA or DEXA) or bone densitometry.
Does osteomalacia cause hypocalcemia?
A common cause of osteomalacia in adults and the elderly is severe deficiency of vitamin D, which leads to chronic hypocalcemia, hypophosphatemia, and secondary hyperparathyroidism.
Is alkaline phosphatase a liver function test?
An alkaline phosphatase test is used to detect diseases of the liver or bones.
Is alkaline phosphatase elevated in osteomyelitis?
In metastatic and some metabolic bone disease, alkaline phosphatase (ALP), calcium, and phosphate are elevated, but they are within normal limits in osteomyelitis. Blood cultures are positive in only 50% of cases of osteomyelitis.
Why is alkaline phosphatase high in hyperparathyroidism?
Bone ALP is secreted by osteoblast cells. It is involved in the bone formation and skeletal mineralization. PTH stimulates osteoblast activity and thus increases level of ALP in blood (8,9).
Which test is useful in evaluation of secondary causes of osteoporosis?
In any patient suspected of having secondary osteoporosis, most experts recommend evaluation of bone and mineral metabolism with blood tests for calcium, phosphate, alkaline phosphatase, 25-hydroxyvitamin D, parathyroid hormone, liver and kidney function, full blood count and thyroid-stimulating hormone.
What happens when the blood calcium level is too low?
Hypocalcemia, also known as calcium deficiency disease, occurs when the blood has low levels of calcium. A long-term calcium deficiency can lead to dental changes, cataracts, alterations in the brain, and osteoporosis, which causes the bones to become brittle. A calcium deficiency may cause no early symptoms.
What is osteomalacia and rickets?
Osteomalacia is softening of the bones. It most often occurs because of a problem with vitamin D, which helps your body absorb calcium. Your body needs calcium to maintain the strength and hardness of your bones. In children, the condition is called rickets.
How does calcitriol affect blood phosphate levels?
Calcitriol increases renal NPT2a expression and phosphate reabsorption, as well as intestinal NPT2b expression and phosphate absorption. Its positive effect on intestinal and renal phosphate absorptions is counterbalanced by the stimulation of fibroblast growth factor 23 (FGF23) production.
What are the results of a bone density scan?
DXA Scan Results It shows how much higher or lower your bone density is than that of a healthy 30-year-old, the age when bones are at their strongest. The lower your score, the weaker your bones are: T-score of -1.0 or above = normal bone density. T-score between -1.0 and -2.5 = low bone density, or osteopenia.
What distinguishes a diagnosis of osteopenia from osteoporosis?
The difference between osteopenia and osteoporosis is that in osteopenia the bone loss is not as severe as in osteoporosis. That means someone with osteopenia is more likely to fracture a bone than someone with a normal bone density but is less likely to fracture a bone than someone with osteoporosis.
Does a bone scan show arthritis?
The test is very sensitive to any difference in bone metabolism. The ability to scan the entire skeleton makes a bone scan very helpful in diagnosing a wide range of bone disorders, including: Fractures. Arthritis.
What causes low calcium levels?
In hypocalcemia, the calcium level in blood is too low. A low calcium level may result from a problem with the parathyroid glands, as well as from diet, kidney disorders, or certain drugs.
Is osteomalacia a primary deficiency?
In adults, prolonged deficiency of vitamin D (calciferol) can lead to osteomalacia, while lesser deficiency (insufficiency) is associated with various non-specific symptoms.
What causes osteopetrosis?
The X-linked type of osteopetrosis, OL-EDA-ID, results from mutations in the IKBKG gene. In about 30 percent of all cases of osteopetrosis, the cause of the condition is unknown. The genes associated with osteopetrosis are involved in the formation, development, and function of specialized cells called osteoclasts.
How is osteopenia diagnosis?
In order to diagnose osteopenia, your doctor will do a bone density test. Bone density measures bone mass and bone strength. One type of test is a dual-energy X-ray absorptiometry (DEXA or DXA). It measures bone density in your hips, spine, and wrist.
What does demineralization mean?
Demineralization is the process of removing minerals ions from HA crystals of hard tissues, for example, enamel, dentin, cementum, and bone. Restoring these mineral ions again to the HA crystals is called remineralization.
What is osteomalacia and osteoporosis differentiate between the two?
In osteoporosis, the bones are porous and brittle, whereas in osteomalacia, the bones are soft. This difference in bone consistency is related to the mineral-to-organic material ratio.
What is blood test for arthritis?
Blood tests People with rheumatoid arthritis often have an elevated erythrocyte sedimentation rate (ESR, also known as sed rate) or C-reactive protein (CRP) level, which may indicate the presence of an inflammatory process in the body.
What is a bone densitometry DXA?
A bone density scan uses low dose X-rays to see how dense (or strong) your bones are. You may also hear it called a DEXA scan. Bone density scans are often used to diagnose or assess your risk of osteoporosis, a health condition that weakens bones and makes them more likely to break.