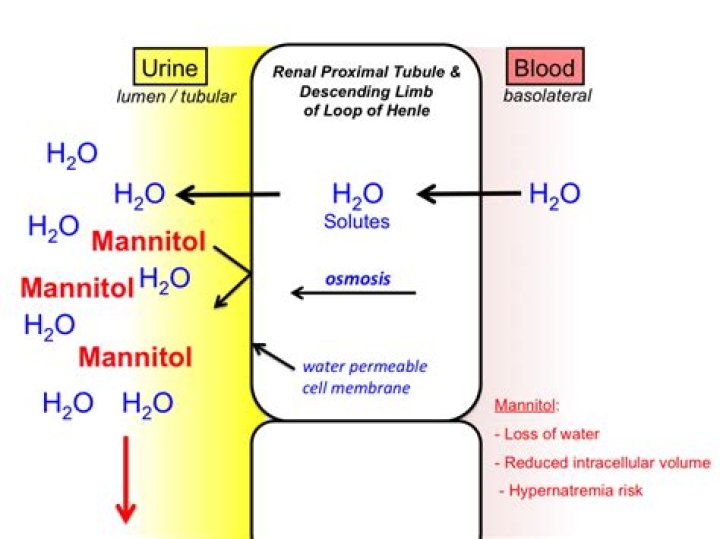
Why is mannitol contraindicated in renal failure
Mannitol therapy should be discontinued if progression in renal damage or dysfunction, heart failure, or pulmonary congestion occurs. A test dose should be administered in patients with severe renal impairment. Diuresis caused by mannitol administration may exacerbate electrolyte imbalances.
Why does mannitol cause renal failure?
Volume depletion and hypernatremia — Mannitol is freely filtered by the glomerulus and does not undergo tubular reabsorption. Thus, it acts as an osmotic diuretic, increasing urinary losses of both sodium and electrolyte-free water.
What medication is contraindicated for renal failure patients?
Problematic drugs whose use in patients with renal insufficiency is nephrologically contraindicated: Pethidine, cefepime, lithium, gilbenclamide, gimepiride, metformin, spironolactone, eplerenone, methotrexate, gadolinium, enoxaparin.
Why is mannitol contraindicated?
OSMITROL Injection (Mannitol Injection, USP) is contraindicated in patients with: Well established anuria due to severe renal disease, Severe pulmonary congestion or frank pulmonary edema, Active intracranial bleeding except during craniotomy, Severe dehydration, Progressive renal damage or dysfunction after …Why mannitol is contraindicated in pulmonary edema?
Mannitol may cause excessive expansion of the intravascular space when administered in high concentrations at a rapid rate. This may result in congestive heart failure and pulmonary edema.
Why mannitol is contraindicated in extradural hematoma?
There is evidence that excessive administration of mannitol may be harmful, by mannitol passing from the bloodstream into the brain, where it increases pressure within the skull and worsens brain swelling.
How does mannitol exacerbate heart failure?
Too rapid infusion of large amounts of mannitol will cause a shift of intracellular water into the extracellular compartment resulting in cellular dehydration and overexpansion of the intravascular space with hyponatremia, congestive heart failure and pulmonary edema.
Is mannitol contraindicated in hemorrhagic stroke?
Mannitol seems safe but might not improve outcome in patients with acute intracerebral hemorrhage.Why is mannitol contraindicated in intracranial hemorrhage?
Therefore, the overall conclusion is that although mannitol decreases edema in ICH at first,[16,17] according to the three following mechanisms, it finally widens ICH, thus, its use is not recommended. There are some of limitation in our study included, lack of sample size and there is no control group.
Is enoxaparin contraindicated in renal failure?The reduced dose enoxaparin is the most robustly studied LMWH regime in patients with renal dysfunction (see table). Care must be taken however to avoid sub-therapeutic treatment in the renal patients.
Article first time published onWhich analgesic is safe in renal failure?
Safe nonopioid options for pain management in renally impaired and dialysis patients include acetaminophen and certain NSAIDs, such as ibuprofen. Fentanyl, hydrocodone, and hydromorphone are the safest opioids to use in renally impaired and dialysis patients.
Is ceftriaxone contraindicated in renal failure?
Ceftriaxone is considered a safe antibiotic for patients with renal insufficiency, since it is excreted via both haptic and renal pathways.
How does mannitol reduce cerebral edema?
Mannitol is the most popular osmotic agent. Osmotic therapy using mannitol reduces ICP by mechanisms that remain unclear. Mannitol is thought to decrease brain volume by decreasing overall water content, to reduce blood volume by vasoconstriction, to reduce CSF volume by decreasing water content.
Is mannitol a potassium sparing diuretic?
Groups commonly used are thiazide diuretics and thiazide-like diuretics (chlorothiazide, chlorthalidone, hydrochlorothiazide, indapamide, and metolazone), loop diuretics (bumetanide, furosemide, and torsemide), potassium-sparing diuretics (amiloride, spironolactone, and triamterene), and osmotic diuretics (mannitol).
Why osmotic diuretics are contraindicated in pulmonary edema?
Although osmotic diuretics are inert, their osmotic properties can induce serious adverse effects. For example, expansion of the extracellular fluid volume by osmotic diuretics may cause heart failure, pulmonary congestion, and pulmonary edema.
Is mannitol contraindicated in hypertension?
Mannitol may worsen intracranial hypertension in patients, especially children, with hyperemia, which can be fatal. Repeated frequent doses of mannitol can leach into the brain and worsen cerebral edema in the long term.
Is mannitol potassium sparing or wasting?
Groups commonly used are thiazide diuretics and thiazide-like diuretics (chlorothiazide, chlorthalidone, hydrochlorothiazide, indapamide, and metolazone), loop diuretics (bumetanide, furosemide, and torsemide), potassium-sparing diuretics (amiloride, spironolactone, and triamterene), and osmotic diuretics (mannitol).
Where does mannitol work in the kidney?
OSMOTIC DIURETICS: MANNITOL Osmotic diuretics are freely filtered at the glomerulus, undergo limited reabsorption by the renal tubule, and are relatively inert pharmacologically. They act primarily at the loop of Henle, and also on the proximal tubule, by extracting water from intracellular compartments.
Is mannitol contraindicated in EDH?
Use of mannitol for controlling increased intracranial pressure (ICP) upon the arrival at emergency department was higher in the patients with poor outcome (10/14, 71.43%). On the other hand, those with good outcome received no treatment of mannitol for EDH (29/60, 48.33%).
Does mannitol increase urine output?
Mannitol increased urine flow by 61% (P < 0.001). This was accompanied by a 12% increase in RBF (P < 0.05) and a 13% decrease in renal vascular resistance (P < 0.05). Mannitol increased the RBF/cardiac output (CO) relation (P = 0.040).
Why mannitol is given?
Mannitol is a diuretic used to force urine production in people with acute (sudden) kidney failure. Mannitol injection is also used to reduce swelling and pressure inside the eye or around the brain.
Why is mannitol contraindicated in acute tubular necrosis?
Once acute tubular necrosis has occurred, mannitol is contraindicated. When mannitol is administered intravenously it becomes distributed in the extracellular fluid within 1 hour, but does not enter the cells.
Is mannitol contraindicated in sah?
There is no evidence of benefit of the administration of mannitol in patients with subarachnoid haemorrhage. However, in patients with signs of rising intracranial pressure and decreasing neurological function the benefits may be felt to outweigh the risks. Neurosurgical advice should be sought and followed.
Does mannitol cause hyponatremia or hypernatremia?
Mannitol is freely filtered by the glomerulus and does not undergo tubular reabsorption. Thus, it acts as an osmotic diuretic, increasing urinary loss of both sodium and electrolyte-free water. Lack of replacement of the fluid loss can lead to both volume depletion and severe hypernatremia.
Why is hydralazine contraindicated in stroke?
Despite its effectiveness in lowering BP, hydralazine can increase intracranial pressure (ICP) while simultaneously lowering MAP, leading to decreased perfusion pressure and increasing the risk of ischemia (108).
Is heparin contraindicated for hemorrhagic CVA?
The common practice of administering heparin soon after cardioembolic stroke is associated with an increased risk for serious bleeding, according to an article in the Archives of Neurology. However, it appears that anticoagulation with warfarin therapy may safely begin shortly after stroke.
What medication is contraindicated in a patient with hemorrhagic CVA?
The use of antiplatelet medication after a primary intracerebral hemorrhage (ICH) is commonly perceived as being contraindicated because of the possibility of increasing the risk of further bleeding.
Which anticoagulant is safe in renal failure?
Warfarin remains the first‐line treatment in end‐stage renal disease, although in this case the decision to use or not to use anticoagulation is strictly individualized. Anticoagulation with heparins is safe in nondialysis‐dependent CKD, but remains a challenge in the hemodialysis patients.
What are the contraindications of enoxaparin?
- Known hypersensitivity to enoxaparin (urticaria, anaphylactic reactions) or any heparin products.
- Active major bleeding such as gastrointestinal bleed.
- History of heparin-induced thrombocytopenia within the past 100 days.
- Active gastric or duodenal ulcers.
- Hemorrhagic cerebrovascular accident.
Can you use LMWH in renal failure?
Background: Low-molecular-weight heparins (LMWH) have been shown to be safer, more effective and more convenient than unfractionated heparin (UFH) in many clinical situations. However, their use is limited in patients with renal insufficiency (RI) due to bioaccumulation.
Which Nsaid is safe in CKD?
What analgesics are safe for people who have kidney disease? Acetaminophen remains the drug of choice for occasional use in patients with kidney disease because of bleeding complications that may occur when these patients use aspirin.