When a pediatric patient is suffering from dehydration the standard fluid bolus is
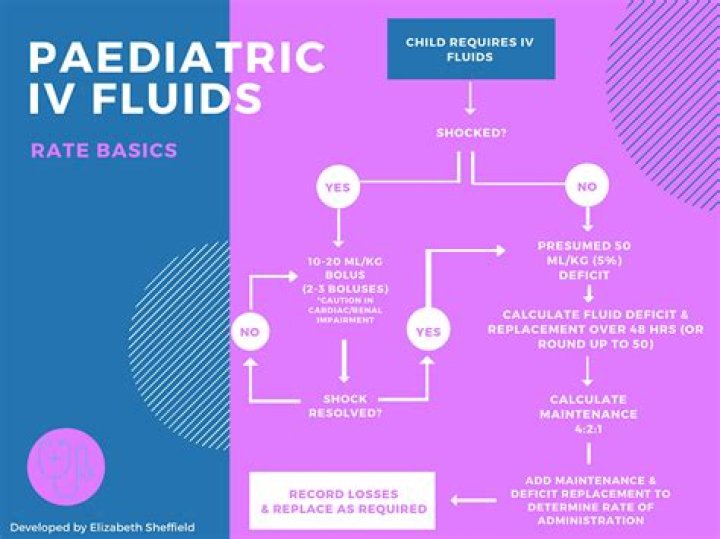
Bolus fluids should be isotonic; either normal saline or lactated ringers solution is used at a volume of 20 mL per kg, given over 60 minutes.
What type of fluid bolus should be given to a dehydrated child?
Isotonic fluid boluses (NS) are the initial approach to the child with moderate to severe dehydration. A bolus is 20 ml/kg (maximum 1 liter). This is typically given over 20 minutes in the child with moderate dehydration and as fast as possible in the child with severe dehydration.
Which IV fluid is best for dehydration?
Hypotonic: The most common type of hypotonic IV fluid is called half-normal saline — which contains 0.45% sodium chloride and 5% glucose . This type is often used to treat dehydration from hypernatremia, metabolic acidosis, and diabetic ketoacidosis.
What is a normal fluid bolus?
The median fluid bolus was 500 ml (range 100 to 1,000 ml) administered over 30 minutes (range 10 to 60 minutes) and the most commonly administered fluid was 0.9% sodium chloride solution.Which is the ideal IV fluid in children?
1. If children and young people need IV fluid resuscitation, use glucose-free crystalloids that contain sodium in the range 131–154 mmol/litre, with a bolus of 20 ml/kg over less than 10 minutes.
What happens if a child is dehydrated?
Lack of Body Fluid A dehydrated baby or toddler will have a reduction in body fluid, which leads to a dry mouth, decreased urine, sunken eyes, and no tears when crying.
What is dehydration in Pediatrics?
The World Health Organization defines dehydration as a condition that results from excessive loss of body water. The most common causes of dehydration in children are vomiting and diarrhea.
How much IV fluid is given for dehydration?
The fluid deficit in severe dehydration equals about 10% of body weight (i.e., 100 ml/kg). Infants should be given IV fluid at a rate of 30 ml/kg in the first hour, followed by 70 ml/kg in the next 5 hours, thus providing a total of 100 ml/kg in 6 hours.Why do you give fluid bolus?
positive fluid balance (associated with worse mortality in AKI, and slower recovery in ARDS) impaired gas exchange (increased extravascular lung water) organ and tissue oedema. acid-base disturbances.
How does a bolus work?In medicine, a bolus (from Latin bolus, ball) is the administration of a discrete amount of medication, drug, or other compound within a specific time, generally 1–30 minutes, in order to raise its concentration in blood to an effective level.
Article first time published onWhy are dehydrated patients given saline?
The simplest approach is to replace dehydration losses with 0.9% saline. This ensures that the administered fluid remains in the extracellular (intravascular) compartment, where it will do the most good to support blood pressure and peripheral perfusion.
How does liquid IV hydrate?
Liquid I.V.’s Cellular Transport Technology uses a specific ratio of potassium, sodium, and glucose to deliver water and other key nutrients directly to your bloodstream. It hydrates you 2-3x faster and more efficiently than water alone.
What IV fluid is appropriate for a bolus to a pediatric patient?
Bolus fluids should be isotonic; either normal saline or lactated ringers solution is used at a volume of 20 mL per kg, given over 60 minutes.
Which assessment is most relevant to the care of an infant with dehydration?
Clinical assessment of dehydration can be difficult, especially in young infants, and rarely predicts the exact degree of dehydration accurately. The most useful individual signs for predicting 5% dehydration in children are an abnormal capillary refill time, abnormal skin turgor and abnormal respiratory pattern.
How do you treat dehydration in babies?
- Give extra fluids in frequent, small sips, especially if the child is vomiting.
- Choose clear soup, clear soda, or Pedialyte, if possible.
- Give popsicles, ice chips, and cereal mixed with milk for added water or fluid.
- Continue a regular diet.
What causes dehydration in infants?
Babies and toddlers can sometimes get a little dehydrated because of their small size. This can happen when they lose water too quickly from vomiting or diarrhea. Dehydration can also happen when babies aren’t getting enough liquids through normal feeding.
When does a toddler become dehydrated?
When to see a doctor if your toddler is dehydrated there’s blood in your toddler’s stool or vomit. your child refuses to drink or have an oral rehydration solution. your toddler’s vomiting or diarrhea is persistent and severe and they can’t drink enough fluid to keep up with how much they’re losing.
What are the symptoms of dehydration?
- Dry mouth and tongue.
- No tears when crying.
- No wet diapers for three hours.
- Sunken eyes, cheeks.
- Sunken soft spot on top of skull.
- Listlessness or irritability.
What are the 5 signs of dehydration?
- Thirst.
- Dry or sticky mouth.
- Not peeing very much.
- Dark yellow pee.
- Dry, cool skin.
- Headache.
- Muscle cramps.
What causes dehydration?
Causes of dehydration Dehydration is caused by not drinking enough fluid or by losing more fluid than you take in. Fluid is lost through sweat, tears, vomiting, urine or diarrhoea. The severity of dehydration can depend on a number of factors, such as climate, level of physical activity and diet.
What best assesses a child's response to each fluid bolus?
The child’s response to each fluid bolus should dictate the course of further treatment. Each bolus should be given over 5-10 minutes and reevaluation should take place.
How do you calculate dehydration fluids?
- Less than 10 kg = 100 mL/kg.
- 10-20 kg = 1000 + 50 mL/kg for each kg over 10 kg.
- Greater than 20 kg = 1500 + 20 mL/kg for each kg over 20 kg.
How do you calculate IV fluid rate for pediatrics?
- For infants 3.5 to 10 kg the daily fluid requirement is 100 mL/kg.
- For children 11-20 kg the daily fluid requirement is 1000 mL + 50 mL/kg for every kg over 10.
- For children >20 kg the daily fluid requirement is 1500 mL + 20 mL/kg for every kg over 20, up to a maximum of 2400 mL daily.
When is bolus insulin given?
Bolus insulin needs to act quickly and so short acting insulin or rapid acting insulin will be used. Bolus insulin is often taken before meals but some people may be advised to take their insulin during or just after a meal if hypoglycemia needs to be prevented.
What is bolus digestive system?
bolus, food that has been chewed and mixed in the mouth with saliva. Chewing helps to reduce food particles to a size readily swallowed; saliva adds digestive enzymes, water, and mucus that help chemically to reduce food particles, hydrate them for taste, and lubricate them for easy swallowing.
How fast can you Bolus normal saline?
A 20 mL/kg 0.9% normal saline bolus (maximum 999 mL) will be administered over 1 hour. This will be followed by D5-0.9% normal saline at a maintenance rate (maximum 55 mL/hr). A 60 mL/kg 0.9% normal saline bolus (maximum 999 mL) over 1 hour will be administered.
What is liquid IV used for?
Quench your thirst and experience effective rehydration fast with Liquid IV Hydration Multiplier Lemon Lime Clean Electrolytes. This refreshing non-GMO electrolyte drink delivers three times the electrolytes of regular sports drinks and gets hydration into your bloodstream more efficiently than just water.
Is liquid IV Safe for Babies?
Q: Can kids drink Liquid I.V.? A: Yes, and they’ll love it!
What is in liquid IV?
What is in Liquid IV? Liquid IV contains a specific ratio of sodium, glucose, and potassium, as well as B-vitamins and vitamin C. It has 3x the electrolytes of traditional sports drinks with less than half the sugar and calories.
What are the 3 main types of IV fluids?
- Isotonic Solutions. Isotonic solutions are IV fluids that have a similar concentration of dissolved particles as blood. …
- Hypotonic Solutions. Hypotonic solutions have a lower concentration of dissolved solutes than blood. …
- Hypertonic Solutions.
How do you assess dehydration in Pediatrics?
The most useful individual signs for identifying dehydration in children are prolonged capillary refill time, abnormal skin turgor, and abnormal respiratory pattern. However, clinical dehydration scales based on a combination of physical examination findings are better predictors than individual signs.